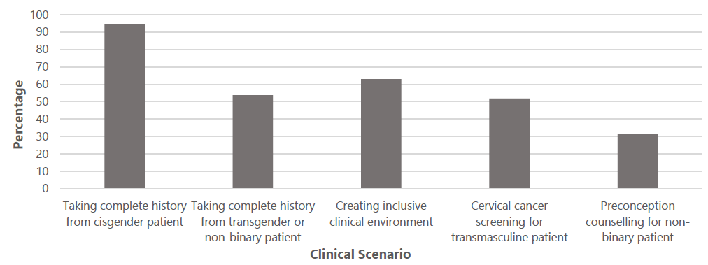
Percentage of medical students who rate themselves as “prepared” to care for patients in various clinical scenarios.
Kyra L. Bonasia1, Allie Morgan2, Christina Grace Solomon3, Ella A. Damiano4
doi: http://dx.doi.org/10.5195/ijms.2022.1279
Volume 10, Number 1: 63-68
Received 12 11 2021: Rev-request 15 11 2021: Rev-request 01 12 2021: Rev-recd 15 11 2022: Rev-recd 14 01 2022: Accepted 11 01 2022
ABSTRACT
Background:Many transgender patients report avoiding healthcare due to discrimination, lack of provider knowledge, and perceived lower quality of care related to their gender identity. One factor contributing to these disparities may be a lack of preparation in medical school related to gender diversity.
Methods:This cross-sectional survey study assessed third- and fourth-year medical students' self-perceived preparedness to provide medical care for gender diverse patients, at one medical school in the United States. Mixed methods were used with both quantitative analyses and qualitative analyses using grounded theory.
Results:54 of 216 eligible students completed the survey (response rate 25%). 53.7% rated themselves as prepared to take a complete medical history from transgender patients compared to 94.4% for cisgender patients. 51.9% rated themselves as prepared to discuss cervical cancer screening with a transmasculine patient. Only 31.5% rated themselves as prepared to provide inclusive preconception counselling. Concerns included using the wrong language and lacking appropriate medical knowledge. The most cited sources of learning about gender diversity were independent learning and fellow students. Five themes emerged in qualitative analyses, two of which included a request for greater opportunities to practice working with gender diverse patients and longitudinal integration of transgender medicine across the curriculum.
Conclusion:Medical students who completed this survey rated themselves as less prepared to care for gender diverse patients compared to cisgender patients. Their current knowledge was largely based on learning outside of the medical school curriculum. The respondents highlighted many opportunities for improvement in medical school curricula.
Keywords: Undergraduate medical education; Curriculum; Health services for transgender persons.
Many transgender patients report avoiding routine healthcare due to experiences of discrimination, lack of provider knowledge of transgender medicine, and perceived lower quality of care related to their gender identity.1,2 One manifestation of this is in the field of obstetrics and gynecology, where transgender and gender diverse individuals experience lower rates of cervical cancer screening and report challenges in accessing reproductive healthcare.1,3-5
One factor that may contribute to these disparities is the lack of formal training that medical students receive during their preclinical and clinical education.6,7 A survey of Canadian and American medical school deans found that a median of five hours was dedicated to “lesbian, gay, bisexual, and transgender-related content” throughout the entire four years of medical school, with significant variation in the quantity, content, and perceived quality of this instruction.6 A recent review found that transgender health content specifically is deficient in medical school curricula, with barriers to incorporation including “limited curricular time, lack of topic-specific competency among faculty, and underwhelming institutional support”.7
Although these reports suggest that gender diversity is not covered adequately in medical school curricula, there is a paucity of information specific to gender diversity content in medical school since it is usually grouped together with sexual orientation content. Furthermore, there is little information on the impact that current curricula have on how prepared students feel to care for patients of diverse gender identities. Our aim was to survey medical students at a single institution, with a goal of assessing their self-perceived preparedness to provide medical care for transgender people, the sources of their learning about gender diversity, and their views on the gender diversity content in their medical school's current curriculum
The STROBE checklist was used as an instrument of evaluation for this cross-sectional survey study.8 The survey was conducted at the Geisel School of Medicine at Dartmouth College in Hanover, New Hampshire, USA. The study was approved by the Dartmouth College Committee for the Protection of Human Subjects (#32109). All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional research committee.
Survey recipients included all third- and fourth-year medical students at the Geisel School of Medicine. Students received an invitation to participate in the study via an email that included a link to an anonymous survey administered through REDCap. After clicking on the link to the anonymous survey, participants were provided with a description of the survey, reminded of their right to not answer any or all of the questions, that they could withdraw at any time, and told “Proceeding with the survey will be taken as consent for participation”. All responses were collected from July 22 to July 31, 2020.
The survey (Supplementary Material) included three respondent demographic questions, five questions with Likert scale responses, one multiple choice question, and two free-text short answers. The questions included five clinical scenarios which asked respondents to rate their level of preparation for each encounter type on a Likert scale from “1 = not prepared at all” to “5 = completely prepared and confident”. The one multiple-choice question asked respondents to cite their sources of learning about gender medicine including pre-clinical education, clinical training including clerkships, fellow medical students, independent learning, or none if they felt they did not learn about gender diversity. Respondents were able to select more than one answer in this category. The free-text questions asked for thoughts on the current curriculum and recommendations for future changes.
In the analysis, respondents were considered “prepared” if they selected either “4 = prepared but not confident” or “5 = completely prepared and confident.” Statistical analyses were performed using a chi-squared test with statistical significance set at 0.05 and a relative risk (RR) calculation with a confidence interval of 95% (95% CI). Descriptive statistics were reported as counts and percentages.
Grounded theory was used to analyze qualitative responses.9 The coding was performed using an open technique and in an iterative fashion with constant comparison to identify similarities and differences. Two researchers (ED and KB) independently coded the responses including assignment of themes. All disagreements were settled by consensus.
The survey was completed by 54 out of 216 of eligible students (response rate 25%). Respondents were 37% (n=20) third-year and 63% (n=34) fourth-year students. The respondents' gender identities were 90.7% (n=49) cisgender; 3.7% (n=2) gender diverse including transgender and non-binary; and 5.6% (n=3) preferred not to answer. The respondents' self-reported sexual orientations were 63.0% (n=34) heterosexual; 31.5% (n=17) non-heterosexual including gay, lesbian, bisexual, pansexual, or queer; and 5.6% (n=3) preferred not to answer.
Of the respondents, 53.7% rated themselves as prepared to take a complete medical history from a transgender or non-binary patient compared to 94.4% for a cisgender patient, with a significant difference in self-rated preparedness based on patient gender-category χ2 (1,54) = 23.34, p<.001. Respondents were 1.8 times more likely to rate themselves as prepared to take a complete medical history from a cisgender patient compared to a transgender patient (RR=1.8, 95% CI 1.4-2.3). 51.9% of respondents rated themselves as prepared to discuss cervical cancer screening with a transmasculine patient. Only 31.5% of respondents rated themselves as prepared to provide inclusive preconception counseling to a non-binary patient on testosterone. 63.0% of respondents (n=34) felt prepared to create a gender inclusive clinical environment (Figure 1).
Figure 1.Percentage of medical students who rate themselves as “prepared” to care for patients in various clinical scenarios.

With respect to learning about transgender medicine, 90.7% of respondents (n=49) selected “independent learning” as one of the sources from which they learned the most about gender diversity, making it the most cited source of learning. The second most cited source of learning was “fellow medical students”, selected by 83.3% (n=45) of respondents. The preclinical curriculum was cited as a source of learning by 42.6% (n=23) of respondents. All clerkships combined were cited 18 times, with Obstetrics and Gynecology selected most often, by 11.1% (n=6) of respondents.
For the free-text responses, five major themes were identified. These included: (1) lack of prioritizing gender diversity content or incorporating it into the official curriculum, (2) recommendations for increased opportunities to practice clinical interactions with gender diverse patients, (3) lack of transgender medicine knowledge of educators, (4) expressions of the importance of this content, and (5) appreciation for direct interactions with gender diverse patients.
Examples demonstrating lack of prioritizing gender diversity content include, “I don't think I ever heard a faculty really acknowledge the importance of recognizing gender diversity as a natural part of Ob/Gyn [or] preventive health care” and “this is one of those topics that USMLE doesn't emphasize.” Another respondent stated, “There was one lecture…and that was it, instead of being integrated into the curriculum ensuring repeated exposure as it should be.”
Suggestions for improvement in the curriculum include, “I'd love to see it integrated more thoroughly into the curriculum both preclinical and clinical” and “test questions where the patient is gender non-conforming and they have a knee problem (or something else irrelevant). I'd love to see it as just another patient identifier so as to normalize gender non-conforming people existing.”
Many respondents expressed a desire for more opportunities to integrate practice with gender diverse patients across the curriculum. “More case-based learning would be very helpful”, stated one respondent. Objective structured clinical examinations (OSCEs) were mentioned frequently as an opportunity to integrate interactions with gender diverse patients during preclinical training. For example, respondents wrote, “we should have an OSCE where we work with a patient who is transgender or gender diverse” and “I would really appreciate simulations with standardized patients where we get to practice interviewing a patient whose gender identity does not correspond to their sex assigned at birth.” Another respondent stated, “I think it would be helpful to practice using [pronouns], maybe with question stems or role playing.”
Multiple respondents commented that their teaching faculty did not seem comfortable with transgender medicine. For example, one respondent stated, “I think many [faculty] are still uncomfortable regarding gender diversity due to not feeling like they know enough or it just being a ‘foreign' topic to them.” Another respondent stated that the longitudinal clinical skills course “would also be a fantastic opportunity to bring… facilitators up to speed (no excuse to say they just ‘don't know' when they are required to cover this material with students).”
With respect to the importance of this content, a respondent wrote that the institution “should be more proactive in teaching students about gender diversity because without it, there is a risk of perpetuating negative stereotypes and false beliefs.” Other respondents stated, “I do not think I have the appropriate knowledge and skill to help [gender diverse people] in the health issues they face” and “If we really want to be training medical professionals [to be] fully competent in basic medical care, we need to take the time to understand how gender diversity…affects every medical field.”
Respondents who were able to learn directly from transgender patients commented on it being a valuable experience. One respondent shared “I greatly appreciated being able to spend some time in an Ob/Gyn transgender medicine clinic.” A preclinical panel with transgender people was also brought up frequently, for example: “the panel members were incredible speakers and their stories were important” and “having guest speakers who discussed their experiences being trans was a great privilege.”
In this cross-sectional survey of third- and fourth-year medical students, respondents identified that they felt less prepared to care for gender diverse patients when compared to cisgender patients. Respondents felt least prepared to provide preconception counseling, while a slight majority felt prepared to create an inclusive clinical environment and to discuss cervical cancer screening. These rates of preparedness are lower than would be expected for students in their final years of undergraduate medical education. The difference in preparedness with respect to obtaining an inclusive history is particularly notable since this is a fundamental skill in clinical education. A lack of comfort with this skill may further perpetuate inequalities in care for gender diverse people.
In the free response, concerns included using the wrong language and lacking appropriate medical knowledge. Respondents voiced concern that their faculty were not knowledgeable in this field of medicine. This lack of faculty knowledge represents a major challenge to educating the next generation of physicians and could be improved with focused continuing medical education.
Based on these survey results, three recommendations can be made to improve undergraduate medical student curricula. First, curricula can incorporate more practice interacting with gender diverse standardized patients including eliciting and using appropriate pronouns and anatomical language, creating an inclusive clinical space, and obtaining an inclusive sexual and reproductive history. Next, gender diversity topics can be integrated longitudinally across pre-clinical blocks. Lastly, testing should normalize gender diverse patients in questions and simulated patient encounters. These recommendations are consistent with evidence that integrating didactic sessions and standardized patient encounters related to lesbian, gay, bisexual, and transgender patients can improve clinical competency in undergraduate medical students.10
Of note, there are institutions which have made substantial advances in integrating this content into their curricula. For example, some institutions include introductory courses on gender identity and sexual orientation, and electives that focus on endocrine care for transgender patients.11, 12 These institutions may serve as role models for others in the pursuit of providing excellent LGBTQ+ training to pre-clinical and clinical students. The American Medical Association also offers free CME hours related to sexual and gender minorities which could be useful for academic faculty and students alike.13
A strength of this study was that is directly surveyed students who had completed the pre-clinical curriculum, with many respondents having completed their core clinical clerkships as well. Another strength of the study is that open-ended qualitative responses were obtained, providing a window into student experiences and views. A limitation of this study was that it reports self-perceived preparedness, which may not correlate with students' objective performance in patient care. Additionally, this was a convenience sample with a lower response rate, therefore there may be selection bias in the respondents who chose to participate.
This study is also limited in that it only reflects experiences from one institution. These results, however, are consistent with other studies that identified a lack of transgender content across other medical school curricula in North America, suggesting that these findings may be generalizable to other American institutions.6,7 Additional research is necessary to assess preparation of medical students in transgender medicine both nationally and internationally.
In conclusion, many medical students in their third and fourth years of training rate themselves as less prepared to care for transgender patients compared to cisgender patients, with most of their learning about gender diversity coming from independent learning or fellow medical students rather than the official medical school curriculum. This perceived lack of preparation may negatively impact our next generation of physicians in their care for gender diverse people. This study may help institutions examine their medical school curricula and make improvements to foster an inclusive and effective training environment with respect to gender medicine.
The authors gratefully acknowledge Paul Hanissian MD for his comments on a draft of this manuscript.
The Authors have no funding, financial relationships or conflicts of interest to disclose.
Conceptualization, Data Curation, Methodology, Project Administration, Resources, Validation, Visualization, Writing – Review & Editing: KLB, AM, GCS, EAD. Investigation: KLB, AM, GCS. Supervision: EAD. Formal Analysis, Writing – Original Draft Preparation: KLB & EAD.
1. James S, Herman JL, Rankin S, Keisling M, Mottet L, Anafi M. The report of the 2015 U.S. Transgender Survey. 2016. Washington DC: National Center for Transgender Equality.
2. Liszewski W, Peebles JK, Yeung H, Arron S. Persons of Nonbinary Gender - Awareness, Visibility, and Health Disparities. N Engl J Med. 2018;379(25):2391-2393.
3. Light AD, Obedin-Maliver J, Sevelius JM, Kerns JL. Transgender men who experienced pregnancy after female-to-male gender transitioning. Obstet Gynecol. 2014;124(6):1120-1127.
4. Peitzmeier SM, Bernstein IM, McDowell MJ, Pardee DJ, Agenor M, Alizaga NM, et al. Enacting power and constructing gender in cervical cancer screening encounters between transmasculine patients and health care providers. Cult Health Sex. 2020;22(12):1315-1332.
5. Stewart T, Lee YA, Damiano EA. Do Transgender and Gender Diverse Individuals Receive Adequate Gynecologic Care? An Analysis of a Rural Academic Center. Transgend Health. 2020;5(1):50-58.
6. Obedin-Maliver J, Goldsmith ES, Stewart L, White W, Tran E, Brenman S, et al. Lesbian, Gay, Bisexual, and Transgender–Related Content in Undergraduate Medical Education. JAMA. 2011;306(9):971-977.
7. Dubin SN, Nolan IT, Streed CG, Greene RE, Radix AE, Morrison SD. Transgender health care: improving medical students' and residents' training and awareness. Adv Med Educ Pract. 2018;9:377-391.
8. Gharaibeh A, Koppikar S. Bonilla-Escobar FJ. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) in the International Journal of Medical Students. Int J Med Stud. 2014;2(2):36-37.
9. Glaser B, Strauss A. The discovery of grounded theory; strategies for qualitative research. Chicago: Aldine Pub. Co. 1967.
10. Sequeira GM, Chakraborti C, Panunti BA. Integrating Lesbian, Gay, Bisexual, and Transgender (LGBT) Content Into Undergraduate Medical School Curricula: A Qualitative Study. Ochsner J. 2012;12(4):379-382.
11. “LGBTQ+ Curriculum” University of Maryland School of Medicine. https://www.medschool.umaryland.edu/LGBTQ-Resources/. Accessed December 14, 2021.
12. University of Pittsburgh School of Medicine. “Diversity, Equity, & Inclusions Mini Electives”. Available from: https://meddiversity.pitt.edu/diversity-mini-electives. Cited December 14, 2021.
13. AMA Ed Hub. “LGBTQ Health, Diversity & Inclusion”. Available from: https://edhub.ama-assn.org/course/265. Cited December 14, 2021.
Kyra L. Bonasia, 1 MD, Ph.D. Geisel School of Medicine, Dartmouth College, Hanover, NH, United States.
Allie Morgan, 2 BA. Geisel School of Medicine, Dartmouth College, Hanover, NH, United States.
Christina Grace Solomon, 3 MD. Geisel School of Medicine, Dartmouth College, Hanover, NH, United States.
Ella A. Damiano, 4 MD. Geisel School of Medicine, Dartmouth College, Hanover; Department of Obstetrics and Gynecology, Dartmouth Hitchcock Medical Center, Lebanon, NH, United States.
About the Author Kyra Bonasia graduated with her MD from the Geisel School of Medicine at Dartmouth, class of 2021 (Hanover, USA). She previously completed her PhD in Psychology from the University of Toronto.
Correspondence: Kyra L. Bonasia. Address: Geisel School of Medicine, Dartmouth College, Hanover, NH, USA. Email: kbona071@uottawa.ca
Editor: Francisco J. Bonilla-Escobar Student Editors: Johnmark Boachie, Joseph Tonge Copyeditor: Joseph Tonge Proofreader: Marcel Chee Layout Editor: Lina Hemmeda Process: Peer-reviewed
Cite as: Bonasia, KL, Morgan A, Solomon GC, Damiano EA. Assessing Medical Students' Self-Perceived Preparedness to Care for Gender Diverse Patients: A Survey Study. Int J Med Stud. 2022 Jan-Mar;10(1):63-68.
Supplementary MaterialSurvey to Assess Medical Students' Self-Perceived Preparedness to Care for Gender Diverse Patient.
| As a reminder, all information in this survey is anonymous, all questions are optional, and you are free to withdraw from the survey at any time before submission without your answers being recorded (simply exit the survey window). This survey should take 10 minutes or less. | |||||
| 1. Which of the following best describes your year / clerkship experience in medical school? |
|
||||
| 2. How prepared do you feel to take a complete medical history (a history you might take at a general new patient visit) from a patient whose gender identity corresponds to their sex assigned at birth? | 1=not prepared at all | 2=mostly unprepared, some idea of where to start | 3=somewhat prepared | 4=prepared but not confident | 5=completely prepared and confident |
| 3. How prepared do you feel to take a complete medical history from a patient whose gender identity does not correspond to their sex assigned at birth (for example gender non-binary, gender-queer, transgender)? | 1=not prepared at all | 2=mostly unprepared, some idea of where to start | 3=somewhat prepared | 4=prepared but not confident | 5=completely prepared and confident |
| 4. How prepared do you feel to create an inclusive clinical environment for patients of any gender identity (for example, working with others to ensure clinic space is inclusive, asking for and using preferred names and pronouns, using gender-neutral language during a medical interview)? | 1=not prepared at all | 2=mostly unprepared, some idea of where to start | 3=somewhat prepared | 4=prepared but not confident | 5=completely prepared and confident |
| 5. From what sources do you feel you learned the most with respect to gender diversity? (Select all that apply.) |
|
||||
| The following are meant as general scenarios that one might encounter as a medical student, to assess how prepared you feel to provide inclusive care for patients who identify with a gender different from their sex assigned at birth. | |||||
| 6. You are a medical student meeting a new patient. He is a 27-year-old transgender male receiving testosterone therapy who just moved to the area. As part of the visit you will be taking a history and recommending relevant screening and vaccinations. You notice from reading his records that he is listed as "overdue for cervical cancer screening. On a scale of 1-5. how prepared do you feel to take an appropriate history and to make recommendations regarding screening and vaccinations? | 1=not prepared at all | 2=mostly unprepared, some idea of where to start | 3=somewhat prepared | 4=prepared but not confident | 5=completely prepared and confident |
| 7. You are a medical student scheduled to see a 30-year-old gender non-binary patient on testosterone. You see from reading back through the medical record that they had been considering pregnancy when they were last seen for a visit 6 months ago. On a scale of 1-5. how prepared do you feel to provide inclusive preconception care for this patient? | 1=not prepared at all | 2=mostly unprepared, some idea of where to start | 3=somewhat prepared | 4=prepared but not confident | 5=completely prepared and confident |
| 8. If you would like to share any other thoughts or perceptions regarding education about gender diversity at Geisel, please do so here: __________________________________________________________________________________________________________________________________________________ | |||||
| 9. If you have any recommendations regarding what you would like to see in medical education about gender diversity, please share them here: ____________________________________________________________________________________________________________________________________________ | |||||
| 10.1f you are comfortable doing so, please select the category of gender identity
that most closely aligns with your gender. ❑ Cisgender ❑ Transgender ❑ Non-binary ❑ Gender-queer ❑ Other, which:_______________ ❑ Prefer not to answer |
|||||
| 11. If you are comfortable doing so, please share how you would describe your sexual
orientation. ❑ Heterosexual/straight ❑ Bisexual ❑ Pansexual ❑ Gay ❑ Lesbian ❑ Queer ❑ Asexual ❑ Other, which: _______________ ❑ Prefer not to answer |
|||||
Copyright © 2022 Kyra L. Bonasia, Allie Morgan, Christina Grace Solomon, Ella A. Damiano
This work is licensed under a Creative Commons Attribution 4.0 International License.
International Journal of Medical Students, VOLUME 10, NUMBER 1, Jan-Mar 2022