Medical Students' Neurodivergent, Disability, and Chronic Illness (NDCI)-Related Perceptions, Knowledge, Knowledge Sources, and Competence.
Emily Hotez1, Maya Ayoub2, Julianna Rava3, Zina Jawadi4, Kashia A. Rosenau5, Lauren Taiclet6, Leane Nasrallah7, Charlotte Poplawski8, Alice A. Kuo9
doi: http://dx.doi.org/10.5195/ijms.2022.1288
Volume 10, Number 2: 148-157
Received 19 11 2021: Rev-request 14 12 2021: Rev-request 11 02 2022: Rev-recd 22 12 2021: Rev-recd 11 02 2022: Accepted 15 04 2022
ABSTRACT
Background:Globally, Neurodivergent, Disability, and Chronic Illness (NDCI) populations face significant health disparities. Lack of physician knowledge about NDCI is a key mechanism underlying these disparities. The current study aimed to describe medical students' perceptions, knowledge, and competence regarding NDCI.
Methods:A cross-sectional study was carried out using an online survey of medical students at a large public university with no NDCI-specific curriculum (n = 97; response rate = 18%). The survey asked about students' perceptions, knowledge, and competence pertaining to NDCI populations.
Results:Most (n = 93, 96%) indicated it is important for physicians to understand the influence of NDCI on patient health and clinical encounters. Yet only seven (7%) and 15 (15%) reported that the NDCI curriculum in their medical school was sufficient, and they felt comfortable taking care of patients with NDCI respectively. Most (n = 87, 90%) wanted their medical school to provide additional NDCI training. Few reported high knowledge about ableism (n = 12, 12%), self-determination (n = 7, 7%), coordinating care (n = 4, 4%) and accommodations (n = 10, 10%). Few indicated high competence in cognitive, physical, social-emotional, and other NDCI types (n = 7 – 32, 7-33%). Existing knowledge often came from personal experiences or the news and media.
Conclusion:Findings demonstrated the gaps in medical education, as exemplified by medical students surveyed in one U.S. public university. Results can inform efforts to ameliorate global health disparities associated with a lack of physician knowledge about NDCI.
Keywords: Medical school; Medical students; Education; Medical education; Disabled persons (Source: MeSH-NLM).
650 million individuals worldwide have a disability, including chronic conditions requiring accommodations, temporary or permanent physical or sensory disabilities, and/or cognitive, educational, and social differences.1 In recognition of the broad spectrum of disability – in alignment with the social model of disability – the current paper refers to these populations as Neurodivergent, Disability, and Chronic Illness (NDCI) populations.2
Despite representing the largest minority group (10% worldwide; 26% nationally), NDCI populations face significant health and healthcare disparities.1,3 They have higher prevalence rates for chronic diseases and lower rates of preventive care utilization relative to non-NDCI populations.4 According to the Centers for Disease Control and Prevention (CDC), one in three NDCI adults does not have a typical healthcare provider and experiences unmet healthcare needs.3 Lower rates of healthcare access begin in childhood and continue throughout their lifetime.5,8 The COVID-19 pandemic highlighted that having an NDCI condition was among the strongest independent risk factors for a COVID-19 diagnosis and COVID-19 mortality.9
Physicians' lack of NDCI knowledge is one mechanism underlying health disparities. Overall, physicians report stress, lack of confidence, fear, and anxiety in providing care for NDCI patients.10 Less than half report high confidence that they can provide quality care to NDCI patients, and many hold biased perceptions of this population.11 Physicians also struggle with navigating key aspects of NDCI patient care, including ableism, self-determination, coordinating care, and accommodations, resulting in a compromise in healthcare quality.12
A lack of knowledge originates from shortcomings in medical education training worldwide.13 For example, only half of U.S. medical school deans report having education curricula about biopsychosocial aspects of caring for patients with NDCI in their schools.14 Indeed, there is a long history of excluding NDCI populations more broadly from conversations about diversity in medical education and society.15 For example, medical education competencies do not specifically identify NDCI conditions,16 and in the instances where an NDCI-focused curriculum is available, content typically focuses on those with physical NDCI conditions.14 Furthermore, competencies do not necessarily translate into changes in curricula. As a result, medical students often graduate without the capacities needed to treat NDCI patients.
Improving physician knowledge and competence by exploring opportunities to provide education to medical students may address health disparities for this population. This study aims to describe current medical students' perceptions, self-reported knowledge, and competence related to treating NDCI patients. Findings have the potential to inform changes to medical school curricula that can ameliorate health disparities for NDCI populations.
The current study was cross-sectional and featured the administration of a Qualtrics survey targeting all medical students at a diverse public university in Los Angeles, California (n = 531). The survey was disseminated via email listservs as well as social media and was available for two weeks (05/14/21 – 05/31/21). Recruitment was concurrent with the survey administration during that period. Inclusion criteria included any student currently enrolled in the host institution as a medical student who was at least 18 years old. This information was confirmed in two screening questions on the survey. Any student who did not meet these criteria was redirected to the end of the survey. A priori power analysis (80% 1- β, alpha = 0.05) indicated a recommended sample of approximately 100 participants. This research was approved by the host institution's Institutional Review Board (IRB#21-000798).
Survey development was an iterative and collaborative process among a team of students and faculty affiliated with the host institution. This team included an NDCI-focused medical student organization, internal medicine residents, and physicians with expertise in NDCI. Psychology and public health researchers provided the content and methodological expertise. Several survey developers self-identified as having an NDCI or a close friend or family member with an NDCI. All collaboration took place utilizing virtual tools such as Zoom and Google Docs. The survey domains – self-reported perceptions, knowledge, and competence – were derived from a series of team discussions identifying the key priorities pertaining to working with patients with NDCI. The team cross-checked surveys that assessed similar constructs and adapted items necessary to align the work with ongoing efforts.18 The challenges due to the COVID-19 pandemic required data collection with minimal burden on potential participants. As a result, the team prioritized a survey administration of fewer than 10 minutes.
The final survey (Supplementary Material) included ten Likert Scale questions reflecting self-reported perceptions (Cronbach's alpha = 0.48), knowledge (Cronbach's alpha = 0.85), and competence (Cronbach's alpha = 0.97), as well as background and demographic questions.
Frequency and descriptive statistics were obtained for each survey item utilizing IBM SPSS Statistics, version 28. Perceptions were categorized based on the frequency of responses that indicated strongly or somewhat disagree; neither agree nor disagree; or strongly or somewhat agree. Knowledge was categorized based on responses that indicated the respondent was not or slightly knowledgeable, moderately knowledgeable, or very or extremely knowledgeable. Competence was categorized based on whether respondents indicated they were extremely or somewhat incompetent; neither competent nor incompetent; or extremely or somewhat component. Respondents were asked to select all knowledge sources that applied. Percentages were rounded to the nearest whole number.
The sample featured 97 medical students, yielding a response rate of 18%. As displayed in Table 1, the sample was diverse with respect to race and ethnicity (White: n = 41, 42%; Black: n = 6, 6%; Native American/Alaska Native: n = 1, 1%; Middle Eastern or North African: n = 3, 3%; Two or more races: n = 5, 5%; Hispanic/Latinx: n = 15, 16%) and year in medical school (one: n = 36, 37%; two-three: n = 29, 30%; four+: n = 17, 18%). The majority reported a close friend or family member with an NDCI condition (54%). Self-reported perceptions, knowledge, knowledge sources, and competence related to working with patients with NDCI are presented in Table 2 and Figure 1.
Table 1.Sample Characteristics.
| Variable | n | % |
|---|---|---|
| Race | ||
| White American | 41 | 42 |
| Asian American, Native Hawaiian, or Pacific Islander | 26 | 27 |
| Black or African American | 6 | 6 |
| Two or more races | 5 | 5 |
| Native American or Alaska Native | 1 | 1 |
| Middle Eastern or North African | 3 | 3 |
| I do not wish to answer. | 7 | 7 |
| No response | 8 | 8 |
| Ethnicity | ||
| Not Hispanic/Latinx | 66 | 68 |
| Hispanic / Latinx | 15 | 16 |
| No response | 16 | 17 |
| Close friend or family member with an NDCI | ||
| Yes | 52 | 54 |
| No | 28 | 29 |
| No response | 17 | 18 |
| Year in medical school | ||
| 1 | 36 | 37 |
| 2–3 | 29 | 30 |
| 4+ | 17 | 18 |
| No response | 15 | 16 |
Perceptions, Knowledge, and Competence Related to Working with Patients with NDCI.
| Variable | Strongly / somewhat disagree | Neither agree nor disagree | Strongly / somewhat agree | No response | ||||
|---|---|---|---|---|---|---|---|---|
| Perceptions | n | % | n | % | n | % | n | % |
| The disability-focused curriculum in my medical school is sufficient. | 74 | 76 | 16 | 17 | 7 | 7 | 0 | 0 |
| I feel comfortable taking care of patients with disabilities. | 74 | 76 | 8 | 8 | 15 | 15 | 0 | 0 |
| I would like my medical school to provide additional training about disabilities. | 4 | 4 | 6 | 6 | 87 | 90 | 0 | 0 |
| It is important for physicians to understand the influence of disability on patient health and clinical encounters. | 1 | 1 | 1 | 1 | 93 | 96 | 0 | 0 |
| Not / slightly knowledgeable | Moderately knowledgeable | Very / extremely knowledgeable | No response | |||||
| Knowledge | n | % | n | % | n | % | n | % |
| Ableism and using anti-ableist language1 | 44 | 45 | 34 | 35 | 12 | 12 | 7 | 7 |
| Self-determination for patients with disabilities 2 | 58 | 60 | 26 | 27 | 7 | 7 | 6 | 6 |
| Coordinating care for patients with disabilities 3 | 71 | 73 | 16 | 17 | 4 | 4 | 6 | 6 |
| Accommodations and benefits for individuals with disabilities 4 | 53 | 55 | 28 | 29 | 10 | 10 | 6 | 6 |
| Extremely / somewhat incompetent | Neither competent nor incompetent | Extremely / somewhat competent | No response | |||||
| Competence | n | % | n | % | n | % | n | % |
| Autism spectrum disorder | 46 | 47 | 16 | 17 | 20 | 21 | 15 | 16 |
| ADHD | 29 | 30 | 21 | 22 | 32 | 33 | 15 | 16 |
| Other cognitive disability | 42 | 43 | 25 | 26 | 15 | 15 | 15 | 16 |
| Cerebral palsy | 59 | 61 | 16 | 17 | 7 | 7 | 15 | 16 |
| NDCI requiring the use of a wheelchair | 36 | 37 | 19 | 20 | 27 | 28 | 15 | 16 |
| Other physical disability | 38 | 39 | 24 | 25 | 20 | 21 | 15 | 16 |
| Obsessive compulsive disorder | 43 | 44 | 20 | 21 | 19 | 20 | 15 | 16 |
| Schizophrenia | 41 | 42 | 23 | 24 | 18 | 19 | 15 | 16 |
| Other social, emotional, or mental illness/disability | 27 | 28 | 27 | 28 | 28 | 29 | 15 | 16 |
| Hearing loss | 36 | 37 | 19 | 20 | 27 | 28 | 15 | 16 |
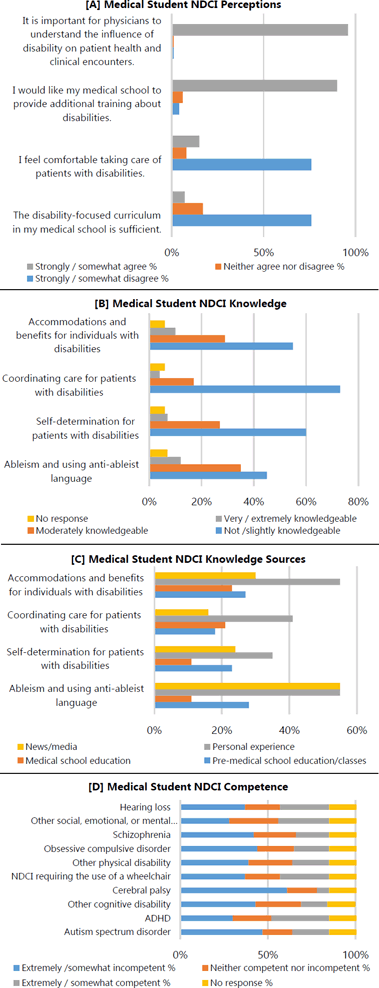
Medical Students' Neurodivergent, Disability, and Chronic Illness (NDCI)-Related Perceptions, Knowledge, Knowledge Sources, and Competence.

Few indicated they strongly or somewhat agreed that the NDCI-focused curriculum in their medical school is sufficient (n = 7, 7%) and that they feel comfortable taking care of patients with NDCI (n = 15, 15%). Most strongly or somewhat agreed that they would like their medical school to provide additional training about NDCI (n=87, 90%) and that physicians need to understand the influence of NDCI on patient health and clinical encounters (n = 93, 96%).
Few indicated that they were knowledgeable about ableism and using anti-ableist language (n = 12, 12%), self-determination for patients with NDCI (n = 7, 7%), coordinating care (n = 4, 4%), and accommodations or benefits (n = 10, 10%) for individuals with NDCI.
Students indicated that the news/media and personal experiences were their primary sources for knowledge on ableism and using anti-ableist language (news/media: n = 53, 55%; personal experience: n = 53, 55%). They were also the primary sources for self-determination (news/media: n = 23, 24%; personal experience: n = 34, 35%) and accommodations and benefits (news/media: n = 30, 30%; personal experience: n = 53, 55%). Most received their knowledge about coordinating care for patients with NDCI from personal experience (n = 40, 41%), followed by medical school education (n = 20, 21%).
Few reported that they were extremely or somewhat competent in caring for individuals with Attention Deficit Hyperactivity Disorder (ADHD, n =32, 33%), other social/emotional/mental illness or disability (n = 28, 29%), hearing loss (n = 27, 28%), NDCI related to using a wheelchair (n = 27, 28%), autism spectrum disorder (n = 20, 21%), other physical disability (n = 20, 21%), obsessive compulsive disorder (n = 19, 20%), schizophrenia (n=18, 19%), other cognitive disability (n = 15, 15%), and cerebral palsy (n = 7, 7%).
This paper describes medical students' self-reported perceptions, knowledge, and competence of working with NDCI populations. The study aligns with previous research that reports a lack of NDCI-specific training during medical school in the U.S. and worldwide.13,19,20 Findings can inform efforts to promote NDCI knowledge and competence among health care workers.
Medical students endorsed the importance of physicians' understanding of NDCI on patient health and clinical encounters. At the same time, most felt that NDCI is insufficiently covered in the curriculum, and they do not feel comfortable caring for patients with NDCI. Most would like their medical school to provide additional training about NDCI. Results support previous findings that medical students require more NDCI training as well as provide new insight into their motivation to receive more substantial training.
In particular, students reported low knowledge about ableism, self-determination, coordinating care, accommodations, and benefits for individuals with NDCI. Existing knowledge on these topics predominantly came from personal experiences or the news and media rather than education or training, reinforcing previously identified gaps in medical training.13,19,20 Few reported high competencies for any of the NDCI conditions asked about on the survey, indicating the need for medical education to provide training on individuals with all NDCI conditions, regardless of support needs or prevalence of the condition.
Gaps in education may be partially due to an under-representation of individuals with NDCI employed in healthcare professions. Three to five percent of medical students disclose an NDCI, which is significantly lower than in the United States (U.S.) NDCI prevalence of 26%.3 It is unclear if this is due to barriers causing underrepresentation in the field or barriers in disclosure and requesting accommodations. Nonetheless, this underrepresentation limits the eventual number of physicians with lived experience managing long-term health conditions, navigating the healthcare system, and requesting accommodations. This, in turn, makes it less likely that NDCI conditions are prioritized in efforts to train the next generation of physicians.
We propose several next steps to address disparities for individuals with NDCI attributable to a lack of physician knowledge. First, we propose that medical schools develop NDCI-focused curricula to foster knowledge and understanding of NDCI and ensure that future doctors can effectively support this population. Following universal design principles, curricula should be multi-modal and integrate discussion-based sessions, didactic materials, and case studies.21 Faculty, administrators, and students should identify practical strategies for implementing this curriculum among the numerous other topics that must be covered in medical school.
Second, there is a need to address barriers to medical school for students with NDCI conditions. Medical student recruitment efforts should prioritize outreach to this population. Concerted efforts should be made within medical schools to ensure all curricula are accessible and provide flexible options for clinical requirements. It should be standard practice that faculty receive NDCI-specific training and collaborate to create a medical school culture that proactively accommodates all students. Third, there is a need to prioritize NDCI-specific education before and after medical school. Efforts before medical school should begin early in development when stigma about NDCI originates, be tailored to children's developmental capacities and be integrated into general educational curricula.22 Efforts after medical school should be integrated into training as Continuing Medical Education. Across all curriculum development efforts, there is a need to collaborate with individuals with NDCI themselves. This is critical to ensure learning objectives, course content, and target outcomes align with their needs, experiences, and priorities.
There were several limitations of this research. Our survey yielded a low response rate relative to the recommended 30% for online surveys.23 Survey administration coincided with the many challenges associated with the ongoing COVID-19 pandemic. Most students reported having a close family member or friend with an NDCI, so responses may have favored those with personal investments in the topic. Response bias may have also favored less comfortable or more dissatisfied with the available NDCI training.24 In addition, the pandemic highlighted and reinforced disparities for NDCI populations, and students may have experienced renewed awareness of these issues.
Further, this research may not be representative of all medical students worldwide. This research was conducted with a small sample of students at a single U.S. institution. Future research should capture a larger and more representative sample and glean cultural and geographic differences. Moreover, there are several emerging medical school initiatives to bolster education on NDCI populations, and results may not apply to institutions that already offer NDCI training.25 In addition, the current study was descriptive and did not rule out the possibility that medical students, in general, may feel less competent in any area of medicine or patient group. NDCI may be one of many inadequately addressed topics in medical education. Future research should investigate whether students' capacities differ significantly for NDCI conditions relative to other conditions.
It should also be noted that this survey was meant to be exploratory and spur additional research; given the constraints presented by the pandemic, we prioritized expedient research methods and design. Future efforts should build on this study by creating a validated tool with robust psychometric properties. Finally, a strength of the survey was that it was developed via a collaborative process among interdisciplinary faculty and students; this survey, however, might not represent the priorities of all faculty and students. Future efforts should involve more extensive collaborations.
This research demonstrates the gaps in medical education pertaining to NDCI populations, as reported by medical students surveyed in one U.S. public university. Results can inform changes to medical school curricula and efforts to ameliorate health disparities associated with a lack of physician knowledge about NDCI.
Medical Students' Perceptions, Knowledge, and Competence in Treating Neurodivergent, Disability, and Chronic Illness (NDCI) Populations: Results from a Cross-Sectional Study.
650 million individuals worldwide have a disability, including chronic conditions requiring accommodations, temporary or permanent physical or sensory disabilities, and/or cognitive, educational, and social differences. In recognition of the broad spectrum of disability – and in alignment with the social model of disability – the current paper refers to these populations as Neurodivergent, Disability, and Chronic Illness (NDCI) populations. NDCI populations face significant health and healthcare disparities. Indeed, having an NDCI condition was among the strongest independent risk factors for a COVID-19 diagnosis and COVID-19 mortality. Physicians lack of knowledge about NDCI – originating from shortcomings in medical training worldwide – is an important mechanism underlying health disparities.
This study aims to describe current medical students' perceptions, self-reported knowledge, and competence related to treating NDCI patients. Findings have the potential to inform changes to medical school curricula that can ameliorate health disparities for NDCI populations.
The current study was cross-sectional and featured the administration of an online survey targeting all medical students at a diverse public university in Los Angeles, California. Survey development was an iterative and collaborative process among a team of students and faculty affiliated with the host institution. The final survey included 10 Likert Scale questions reflecting self-reported perceptions, knowledge, and competence, as well as background and demographic questions. The sample featured a diverse sample of 97 medical students.
Few medical students surveyed indicated that the NDCI-focused curriculum in their medical school was sufficient and reported feeling comfortable taking care of patients with NDCI. Most wanted additional training about NDCI. Few indicated that they were knowledgeable about ableism and using anti-ableist language, self-determination for patients with NDCI, coordinating care, and accommodations or benefits for individuals with NDCI. Existing knowledge about these topics primarily came from the news, media, and personal experiences. When asked about specific NDCI conditions, few students reported that they were extremely or somewhat competent in caring for individuals with each condition.
Findings from this research demonstrate the gaps in medical education, as exemplified by medical students surveyed in one U.S. public university. Results can inform efforts to develop NDCI curricula and ameliorate global health disparities associated with a lack of physician knowledge about NDCI conditions.
The Authors have no financial relationships or conflicts of interest to disclose. This study was partially funded as part of Autism Intervention Research Network on Physical Health (AIR-P Network) by a grant of the Health Resources & Service Administration (HRSA) Maternal & Child Health with grant number UT2MC39440.
Conceptualization: EH, MA, JR, ZJ, KAR, LT, LN, CP, AAK; Data Curation: EH; Formal Analysis: EH, JR; Investigation: EH, AAK; Methodology: EH, MA, JR, ZJ, KAR, LT, LN, CP, AAK; Project Administration: EH, AAK; Resources: AAK; Supervision: EH, MA, AAK; Validation: EH; Writing – Original Draft Preparation: EH, MA, JR, ZJ, LN, CP; Writing – Review & Editing: EH, MA, JR, ZJ, KAR, LT, LN, CP, AAK.
The authors wish to acknowledge the UCLA student organization, DCI at DGSOM (Disability and Chronic Illness at the David Geffen School of Medicine), for their contributions to this research.
1. United Nations. Fact sheet on Persons with Disabilities. Available from: https://www.un.org/disabilities/documents/toolaction/pwdfs.pdf.. Accessed April 7, 2022.
2. Kattari SK, Lavery A, Hasche L. Applying a social model of disability across the life span. J Hum Behav Soc Environ. 2017;27(8):865–80.
3. National Center on Birth Defects and Developmental Disabilities, Centers for Disease Control and Prevention. Disability Impacts All of Us. Available from: https://www.cdc.gov/ncbddd/disabilityandhealth/infographic-disability-impacts-all.html. Published September 16, 2020. Accessed April 7, 2022.
4. Reichard A, Stolzle H, Fox MH. Health disparities among adults with physical disabilities or cognitive limitations compared to individuals with no disabilities in the United States. Disabil Health J. 2011;4(2):59–67.
5. Vohra R, Madhavan S, Sambamoorthi U, St Peter C. Access to services, quality of care, and family impact for children with autism, other developmental disabilities, and other mental health conditions. Autism. 2014;18(7):815–26.
6. Akobirshoev I, Parish S, Mitra M, Dembo R. Impact of Medical Home on Health Care of Children With and Without Special Health Care Needs: Update from the 2016 National Survey of Children's Health. Matern Child Health J. 2019;23(11):1500–7.
7. Cheak-Zamora NC, Thullen M. Disparities in Quality and Access to Care for Children with Developmental Disabilities and Multiple Health Conditions. Matern Child Health J. 2017;21(1):36–44.
8. Cheak-Zamora NC, Yang X, Farmer JE, Clark M. Disparities in transition planning for youth with autism spectrum disorder. Pediatrics. 2013;131(3):447–54.
9. Gleason J, Ross W, Fossi A, Blonsky H, Tobias J, Stephens M. The devastating impact of Covid-19 on individuals with intellectual disabilities in the United States. NEJM Catal Innov Care Deliv. 2021;2(2).
10. Pelleboer-Gunnink HA, Van Oorsouw W, Van Weeghel J, Embregts P. Mainstream health professionals' stigmatising attitudes towards people with intellectual disabilities: A systematic review. J Intellect Disabil Res. 2017;61(5):411–34.
11. Iezzoni LI, Rao SR, Ressalam J, et al. Physicians' Perceptions Of People With Disability And Their Health Care: Study reports the results of a survey of physicians' perceptions of people with disability. Health Aff (Millwood). 2021;40(2):297–306.
12. Kuhlthau KA, Delahaye J, Erickson-Warfield M, Shui A, Crossman M, van der Weerd E. Health care transition services for youth with autism spectrum disorders: Perspectives of caregivers. Pediatrics. 2016;137(Supplement 2):S158–66.
13. Ajuwon PM, Lesi FEA, Odukoya O, Melia C. Attitudes of medical students toward disabilities in Nigeria. Int J Disabil Hum Dev. 2015;14(2):131–40.
14. Seidel E, Crowe S. The State of Disability Awareness in American Medical Schools. Am J Phys Med Rehabil. 2017;96(9):673–6.
15. Andrews EE, Forber-Pratt AJ, Mona LR, Lund EM, Pilarski CR, Balter R. #SaytheWord: A disability culture commentary on the erasure of “disability”. Rehabil Psychol. 2019;64(2):111–8.
16. Association of American Medical Colleges (AAMC). Core Competencies for Entering Medical Students. https://www.aamc.org/services/admissions-lifecycle/competencies-entering-medical-students. Accessed April 7, 2022.
17. Medical School Admission Statistics for UCLA Graduates Dashboards | UCLA Student Affairs Information & Research Office. https://sairo.ucla.edu/amcas. Accessed April 6, 2022.
18. Borowsky H, Morinis L, Garg M. Disability and Ableism in Medicine: A Curriculum for Medical Students. MedEdPORTAL. Published online January 25, 2021:11073.
19. Low HM, Zailan F. Medical students' perceptions, awareness, societal attitudes and knowledge of autism spectrum disorder: an exploratory study in Malaysia. Int J Dev Disabil. Published online December 5, 2016. Accessed April 6, 2022. https://www.tandfonline.com/doi/abs/10.1080/20473869.2016.1264663.
20. Santoro JD, Yedla M, Lazzareschi DV, Whitgob EE. Disability in US medical education: Disparities, programmes and future directions: Health Educ J. Published online June 15, 2017.
21. Scott SS, McGuire JM, Foley TE. Universal design for instruction: A framework for anticipating and responding to disability and other diverse learning needs in the college classroom. Equity Excell Educ. 2003;36(1):40–9.
22. Walker JS, Coleman D, Lee J, Squire PN, Friesen BJ. Children's Stigmatization of Childhood Depression and ADHD: Magnitude and Demographic Variation in a National Sample. J Am Acad Child Adolesc Psychiatry. 2008;47(8):912–20.
23. Yun GW, Trumbo CW. Comparative Response to a Survey Executed by Post, E-mail, & Web Form. J Comput-Mediat Commun. 2000;6(1).
24. Andrews MW. Who Is Being Heard? Response Bias in Open-ended Responses in a Large Government Employee Survey. In: A Section on Survey Research Methods. 2005:7.
25. Havercamp SM, Barnhart WR, Robinson AC, Whalen Smith CN. What should we teach about disability? National consensus on disability competencies for health care education. Disabil Health J. 2021;14(2):100989.
Emily Hotez, 1 Ph.D. University of California, Los Angeles (UCLA), David Geffen School of Medicine, United States.
Maya Ayoub, 2 MD, Ed.M. University of California, Los Angeles (UCLA), David Geffen School of Medicine, United States.
Julianna Rava, 3 MPH. University of California, Los Angeles (UCLA), David Geffen School of Medicine, United States.
Zina Jawadi, 4 MS. University of California, Los Angeles (UCLA), David Geffen School of Medicine, United States.
Kashia A. Rosenau, 5 Ph.D. University of California, Los Angeles (UCLA), David Geffen School of Medicine, United States.
Lauren Taiclet, 6 MS. University of California, Los Angeles (UCLA), David Geffen School of Medicine, United States.
Leane Nasrallah, 7 BS. University of California, Los Angeles (UCLA), David Geffen School of Medicine, United States.
Charlotte Poplawski, 8 BS. University of California, Los Angeles (UCLA), David Geffen School of Medicine, United States.
Alice A. Kuo, 9 MD, Ph.D., MBA. University of California, Los Angeles (UCLA), David Geffen School of Medicine, United States.
About the Author: Zina Jawadi completed her bachelor's and master's degrees at Stanford University, is a second-year medical student at UCLA's David Geffen School of Medicine, and serves on the Board of Directors of the Hearing Loss Association of America.
Correspondence: Emily Hotez, Address: 10833 Le Conte Ave, Los Angeles, CA, 90095, USA. Email: ehotez@mednet.ucla.edu
Editor: Francisco J. Bonilla-Escobar Student Editors: Adam Urback & Brandon Belbeck Copyeditor: Madeleine J. Cox Proofreader: Benjamin Liu Layout Editor: Cesare Mercalli Process: Peer-reviewed
Cite as: Hotez E, Ayoub A, Rava J, Jawadi Z, Rosenau KA, Taiclet L, et al. Medical Students' Perceptions, Knowledge, and Competence in Treating Neurodivergent, Disability, and Chronic Illness (NDCI) Populations: Results from a Cross-Sectional Study. Int J Med Stud. 2022 Apr-Jun;10(2):148-57.
Neurodivergent, Disability, and Chronic Illness (NDCI)Survey
| 1. Are you a current [medical school] student? | □Yes □No |
| 2. Are you at least 18 years or older? | □Yes □No |
| 3. Please indicate the extent to which you aqree/disaqree with the following statements. | |
| The disability-focused curriculum in my medical school is sufficient. |
|
| I feel comfortable taking care of patients with disabilities. |
|
| I feel comfortable conducting all portions of the physical exam and history for a patient with a disability. |
|
| I would like my medical school to provide additional training about disabilities. |
|
| I believe it is important for physicians to understand the influence of disability on patient health and clinical encounters. |
|
| My medical school is supportive of medical students with disabilities. |
|
| 4. Rate your knowledge on the following topics. | |
| Ableism, and using anti-ableist language. |
|
| Self-determination for patients with disabilities. |
|
| Coordinating care for patients with disabilities. |
|
| Health disparities for individuals with disabilities. |
|
| Accommodations and benefits for individuals with disabilities. |
|
| 5. Indicate the source of your knowledge on the following topics (select all that apply). | |
| Ableism, and using anti-ableist language. |
|
| Self-determination for patients with disabilities. |
|
| Coordinating care for patients with disabilities. |
|
| Health disparities for individuals with disabilities. |
|
| Accommodations and benefits for individuals with disabilities. |
|
| 6. Rate how competent/comfortable you feel treating/providing care for an individual with the following disabilities within your intended specialty. | |
| Autism spectrum disorder |
|
| ADD/ADHD |
|
| Other cognitive disability |
|
| Cerebral palsy |
|
| Impairment requiring the use of a wheelchair |
|
| Other physical disability |
|
| Obsessive compulsive disorder |
|
| Schizophrenia |
|
| Other social, emotional, or mental illness/disability |
|
| Hearing loss |
|
| Other (rate/specify if there are other conditions you would like to rate your competence/comfort with) |
|
| 7. Do you or a close friend/family member have a disability? | □Yes □No |
| 8. Please indicate your year in medical school? | □1 □2 □3 □4 □> 4 |
| 9. Are you Hispanic/Latinx? | □Yes □No |
| 10. Please indicate your race (select all that apply) |
|
| End of survey | |
Copyright © 2022 Emily Hotez, Maya Ayoub, Julianna Rava, Zina Jawadi, Kashia A. Rosenau, Lauren Taiclet, Leane Nasrallah, Charlotte Poplawski, Alice A. Kuo
This work is licensed under a Creative Commons Attribution 4.0 International License.
International Journal of Medical Students, VOLUME 10, NUMBER 2, April 2022