Risk Factors associated with the Development of Type II Diabetes Mellitus.
Diego Carrion Alvarez1, Nallely Alejandra Obregon Perales1
doi: http://dx.doi.org/10.5195/ijms.2019.423
Volume 7, Number 3: 97-99
Received 29 08 2019: Rev-recd 19 10 2019: Accepted 01 11 2019
In our university, we started clinical rotations in family medicine. For six months, we learned how to diagnose and treat patients from all socioeconomic classes. However, some cases had an impact on us. A lady in her late 60's came for her routine diabetes check-up. She had been diagnosed just three months ago; currently, she was taking metformin and trying to improve her lifestyle. Her lab tests results were still above the recommended values. Our doctor invited us to ask her about her habits and diet. She did not exercise; furthermore, the nutritionist recommended her a Mediterranean diet. We suggested the idea of starting insulin if her lab results persisted. Her answer shocked us: “Doctors, how am I supposed to change my diet? The plan provided by the nutritionist includes fish and olive oil. I barely have money to buy a few eggs, beans and tortillas, and eat chicken or meat only when possible. Even more, I doubt I could afford the syringes and the needles for the insulin injections.” Our tutor recommended small diet changes and increased the metformin dose. The patient was discharged with a new appointment to review her glucose values. Upon this scenario, we learned what it is like to have a chronic disease as a low-income patient in a middle-income country.
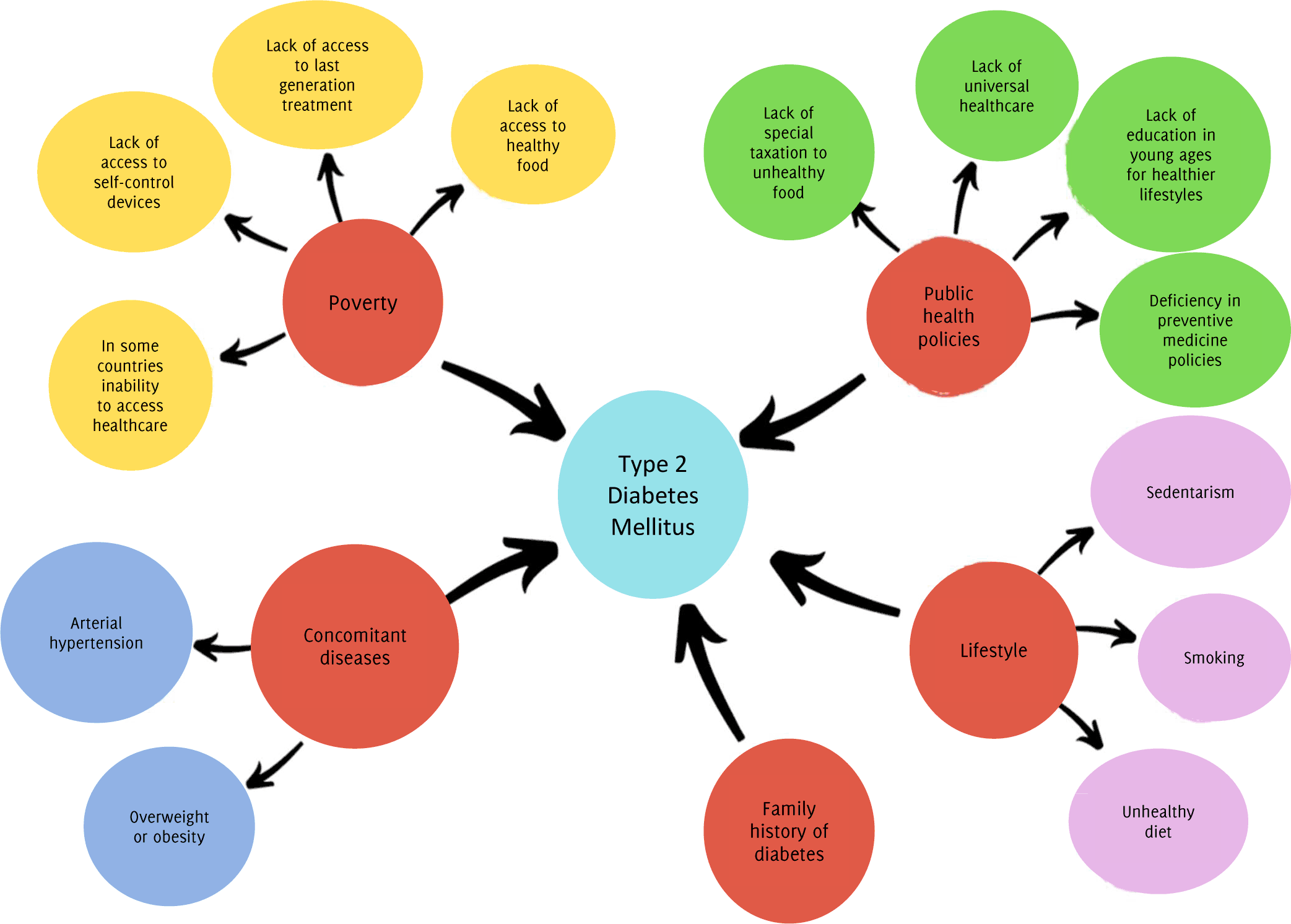
In Mexico, diabetes represents a significant health problem. The current lifestyle, dietary habits, and an alarming increase in obesity rates are just the tip of an underlying issue. In 2012, diabetes prevalence was around 8.9%. However, prospective studies expect it to grow to 22.6% by 2050, meaning that almost one in every three Mexicans will suffer from the disease.1 The picture in Latin America is similar since the prevalence of diabetes has increased by 9% from 2014 to 2016.2 In a country like Mexico, where according to the World Bank 3.2 million inhabitants live with less than 1.90 USD a day and 44.4 million struggle to survive with less than 5.50 USD, it can be difficult to change your lifestyle. Diabetes is a multifactorial disease, and even though poverty plays a significant role in its development, other factors such as governmental policies addressing unhealthy food and encouraging early lifestyle changes contribute to the big picture. These factors are mentioned in Figure 1 and need to be considered when outlining the correct public health approach to the problem.3 Low-income populations tend to have worse outcomes and so they need to be targeted by health institutions.4
Figure 1Risk Factors associated with the Development of Type II Diabetes Mellitus.

Diabetes is one of the most prevalent diseases worldwide. It is a chronic disorder and requires strict control. In 2015, the economic burden of diabetes was estimated at 1.3 trillion USD globally and is estimated to increase up to 2.2 trillion USD by 2030; furthermore, even if countries meet international targets, that will not reduce the burden of the disease.2 Latin American healthcare systems absorb part of the economic charge by providing medical appointments, lab tests and certain medications. However, due to the huge amount of patients and the lack of resources, they are unable to afford the newest medication available, relying on cheaper drug options. Polypharmacy is an important part of diabetes management, and since not all drugs are available, some patients may be unable to reach therapeutic goals, presenting complications or switching to insulin-based treatments.5 Healthcare systems also cover the costs of complications such as neuropathy, retinopathy, nephropathy or limb amputation; these are all complications that impact negatively on the economy taking out of the workforce otherwise productive individuals. Even with these systems, diabetes still represents a cost for the patient; changing to a healthier lifestyle and buying syringes and needles is a patient's responsibility, as well as the acquisition of a glucometer, lancets and paper strips for proper self-management.
It is said that each individual is a world; the personalization of treatment in middle income countries needs to start. Mexican guidelines are outdated, and they stick to the recommendations of the American Diabetes Association (ADA) without considering the differences in our countries healthcare systems, social structure, and economic capabilities. An example of a more personalized adaptation can be found in the 2018 consensus between the ADA and the European Association for the Study of Diabetes (EASD) since in this guideline policymakers do contemplate medicine costs.6 However, contexts are unique to each country and they even vary between regions; Mexican health authorities, such as the “Centro Nacional de Excelencia Tecnológica en Salud”, need to change their approach and focus the attention of protocols also on treatment individualization based on economic status and even the patients’ cooperation. As students, it is our duty to demand better healthcare options for our patients by pushing governmental institutions to shift to a more personalized care and ensure that preventive health policies may endure.
None.
The Authors have no funding, financial relationships or conflicts of interest to disclose.
Conceptualization: DCA, and NAOP. Validation: DCA, and NAOP. Formal Analysis: DCA, and NAOP. Investigation: DCA, and NAOP. Writing – Original Draft: DCA, and NAOP. Writing – Review & Editing: DCA, and NAOP. Supervision: DCA.
1.Meza R, Barrientos-Gutierrez T, Rojas-Martinez R, Reynoso-Noverón N, Palacio-Mejia LS, Lazcano-Ponce E. Burden of type 2 diabetes in Mexico: past, current and future prevalence and incidence rates. Prev Med. 2015 Dec;81:445–50.
2.Arredondo A, Azar A, Recamán AL. Diabetes, a global public health challenge with a high epidemiological and economic burden on health systems in Latin America. Glob Public Health. 2018 Jul;13 (7):780–787.
3.Gaman MA, Dobrica EC, Pascu EG, Cozma MA, Epingeac ME, Gaman AM. Cardio metabolic risk factors for atrial fibrillation in type 2 diabetes mellitus: Focus on hypertension, metabolic syndrome and obesity. J Mind Med Sci. 2019;6(1):157–161.
4.Stevens CD, Schriger DL, Raffetto B, Davis AC, Zingmond D, Roby DH. Geographic Clustering Of Diabetic Lower-Extremity Amputations In Low-Income Regions Of California. Health Aff (Millwood). 2014 Aug;33 (8):1383–90.
5.Dobrica EC, Gaman MA, Cozma MA, Bratu OG, Pantea Stoian A, Diaconu CC. Polypharmacy in Type 2 Diabetes Mellitus: Insights from an Internal Medicine Department. Medicina (Kaunas). 2019Aug3;55 (8). pii: E436.
6.Davies MJ, D'Alessio DA, Fradkin J, Kernan WN, Mathieu C, Mingrone G. Management of Hyperglycemia in Type 2 Diabetes, 2018. A Consensus Report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2018 Dec;41 (12):2669–2701.
Diego Carrion Alvarez, 1 Medical Student, University of Monterrey, Monterrey, Mexico
Nallely Alejandra Obregon Perales, 1 Medical Student, University of Monterrey, Monterrey, Mexico
Mihnea-Alexandru Găman, Editor
About the Author: Diego Carrion is currently a 5th year medical student of Universidad de Monterrey, Monterrey, México of a 7 year program. He is also a recipient of a Millenium Fellowship student fellowship.
Correspondence: Diego Carrion Alvarez, Address: Av. Ignacio Morones Prieto 4500 San Pedro Garza García Nuevo León, México. Email: diego.carrion@udem.edu
Cite as: Carrion Alvarez D, Obregon Perales NA, Having Diabetes in a Middle-Income Country. Int J Med Students. 2019 Sep-Dec;7(3):97-9.
Copyright © 2019 Diego Carrion Alvarez, Nallely Alejandra Obregon Perales
This work is licensed under a Creative Commons Attribution 4.0 International License.
International Journal of Medical Students, VOLUME 7, NUMBER 3, December 2019