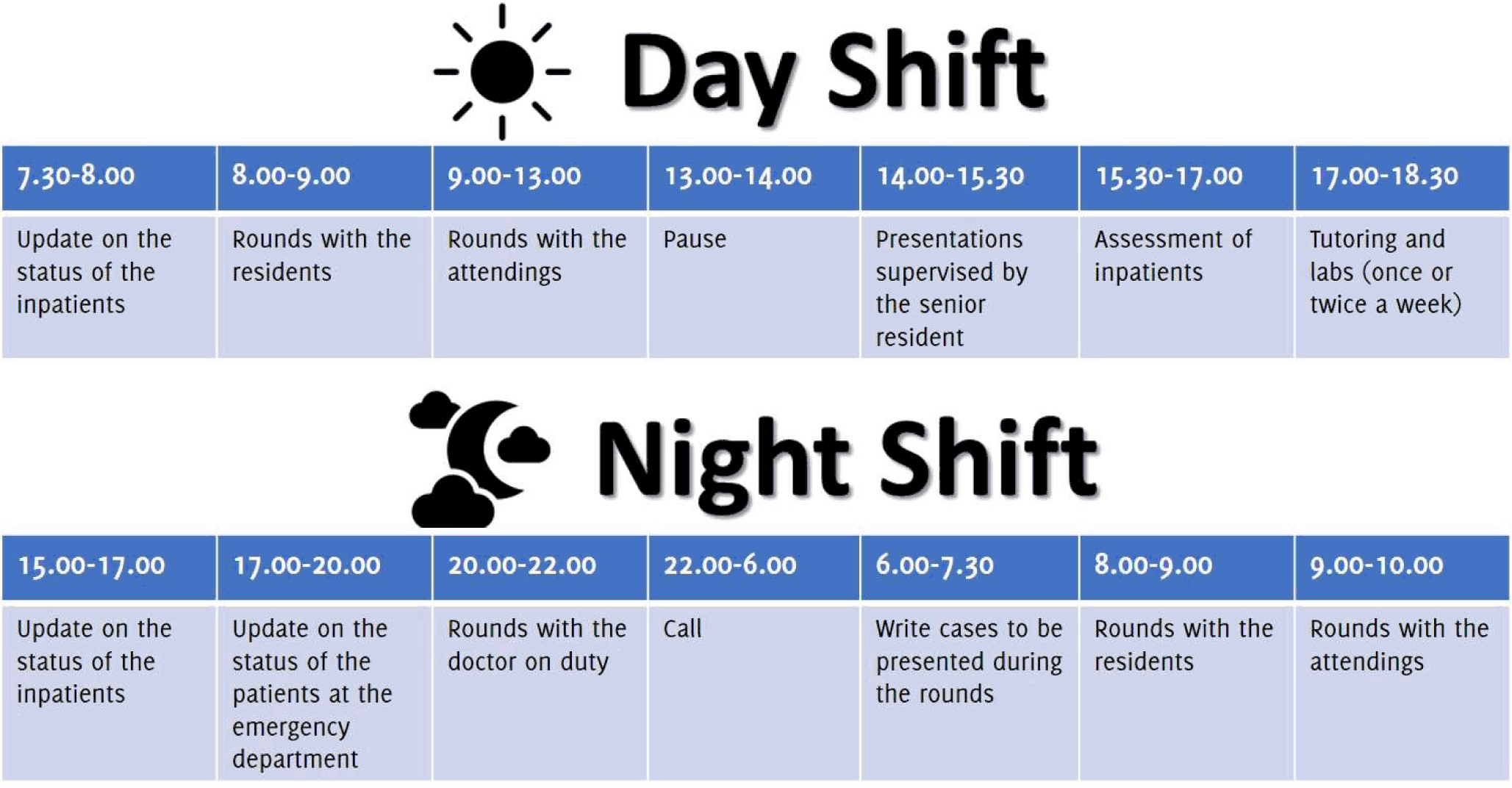
Shift schedule of final year medical students.
Olga Djoutsop Mbougo1, Vanessa Youmbi Nono1, Ulrick S. Kanmounye1
doi: http://dx.doi.org/10.5195/ijms.2020.539
Volume 8, Number 2: 177-179
Received 28 04 2020: Rev-request 29 06 2020: Rev-recd 01 07 2020: Accepted 01 07 2020
Authors ODM and VYN are Cameroonian students in their final year of medical school in the Democratic Republic of Congo (DRC). Both were enrolled initially in Cameroonian medical schools but had to transfer to the DRC after their schools were closed. ODM was in her second year of medical school out of seven years while VYN was in her third year. ODM transferred the same year the schools were closed, while VYN spent a year out of medical school before she transferred. For the two students, the DRC is their new home – it welcomed them when their home would not. In their seventh and final year of medical school, the two are on a twelve-month rotation at the Mother and Infant Monkolé Hospital Center, a 158-bed referral hospital in the capital of the DRC.1
Before ODM and VYN began their rotations, they were apprehensive and lacked certainty. As time went by, they grew professionally and gained confidence. They had a busy seven-day schedule – day shifts, three-night shifts, and one off-duty day (Figure 1). Their interactions with the staff were informative, and most surgical interventions were planned so the students could read up on the cases. The students learned to perform appendectomies, cesarean sections, ultrasonographies, and gastroscopies under the supervision of the senior residents and attendings.
Figure 1.Shift schedule of final year medical students.

On March 10, 2020, the DRC registered their first case of COVID-19 in the region, and it also marked the point in time in which our outlook towards COVID-19 shifted.2 Before the first case of COVID-19, the general feeling was that the diseases affected other countries. Even after the first case was registered in the DRC, we were still unconcerned in our hospital. However, we were proven wrong on March 19, 2020, when we admitted our first COVID-19 case. It was inevitable given that our hospital is one of the premier health facilities in the country. The diagnosis resulted in a panic within the hospital. Confusion and fear replaced the natural feeling of assurance despite the rapid and practical measures that had been put in place.
Fortunately, the hospital leadership responded promptly. The hospital dedicated an entire building to the isolation and quarantine of COVID-19 cases. Also, infrared thermometers and taps were made available in every wing, entrance, and exit points. A work from home protocol was initiated for those whose work did not warrant their physical presence at the hospital, and a new triage protocol was put in place.
We had all been briefed on what to do and when to act. This situation was new but still old. New because of the global reach of COVID-19, and old because we had dealt with epidemics of cholera and Ebola viral disease before.3,4 Inexplicably, though, there was panic. The staff and students were upset that they did not have regular supplies of personal protective equipment (PPE). The hospital administration, unable to get enough PPE, then decided to limit the clinical personnel in-hospital. Although the administration felt the students had a role to play in the COVID-19 response, they made the hard decision to suspend student rotations indefinitely. The students felt helpless; they wished they could help.
On March 19, 2020, the Congolese president announced a national “stay at home” and gave the citizens a couple of days to get provisions. This decision had the undesirable effect of causing stampedes in produce markets and supermarkets. Some cupid traders used price gouging to make the most of their new “business opportunity.” The price gouging led to more panic buying among the high- and middle-class but left the most vulnerable without everyday necessities. These tragic events led to a reversal of the presidential decision and a firm decision by the authorities on unnecessary exposure to COVID-19.5,6
We have been at home, hoping for all of this to come to an end. Staying at home and not being able to help is difficult. We wonder what happened to all those patients who had malaria, typhoid fever, strokes, acute appendicitis, postpartum hemorrhage, and neonatal infections. We do understand that staying at home is the best way we can help right now, given the situation. The last thing we need is for health personnel to be infected in a country with a limited workforce density. So, we are playing our part to the best of our abilities.
Three times a week, we go from one home to another and test patients in the suburbs. We report and isolate suspected cases, and we educate the seronegative entourage on how to interact with their seropositive acquaintance. Besides testing patients, we raise funds and distribute clean water, soap, and hydroalcoholic hand sanitizers. Unfortunately, none of the medical schools are organizing online classes, so we organize weekly group study sessions on Zoom.
Post-COVID, we anticipate there will be an economic crisis. In a country where more than half of the population lives on less than USD $1.90 and where the number of physicians is insufficient,7 this pandemic will push more people into poverty, increase the burden of disease, and decrease the number of physicians.8-10 The personal economy is a major social determinant of health, and the new state of poverty will undoubtedly translate to a new disease burden. As future physicians, we must think about innovative strategies to manage the new disease burden because this is just as important as learning to perform a cesarean section or graduating on time. While at home, we are strengthening our research capacities and reading up on potential solutions to propose measures to combat the spread of COVID-19 to the Congolese people.
Life will no longer be the same, and it is up to us to define what the new “normal” will be.
We wish to thank René Lumu and Wilfrid Mbombo for their material support with this paper.
The Authors have no funding, financial relationships or conflicts of interest to disclose.
Conceptualization, Writing – Original Draft Preparation & Writing – Review & Editing: ODM, VYN, USK.
1.Monkole Mother and Child Hospital Center. Presentation of the Monkole Mother and Infant Hospital Center. Available from: https://monkole.cd/presentation-demonkole/. Last updated May 18, 2018; cited October 20, 2019.
2.World Health Organization. First case of COVID-19 confirmed in the Democratic Republic of the Congo. WHO | Regional Office for Africa. 2020. Available from: https://www.afro.who.int/news/first-case-covid-19-confirmed-democratic-republic-congo. Last updated June 29, 2020; cited July 1, 2020.
3.Ilunga Kalenga O, Moeti M, Sparrow A, Nguyen V-K, Lucey D, Ghebreyesus TA. The Ongoing Ebola Epidemic in the Democratic Republic of Congo, 2018-2019. N Engl J Med. 2019 July;381 (4):373–83.
4.Ingelbeen B, Hendrickx D, Miwanda B, van der Sande MAB, Mossoko M Vochten H . Recurrent Cholera Outbreaks, Democratic Republic of the Congo, 2008–2017. Emerg Infect Dis. 2019 May;25 (5):856–64.
5.Ministry of Health, Democratic Republic of Congo. STOP Coronavirus in DRC. Available from: https://www.stopcoronavirusrdc.info/mesures-de-protection-contre-le-coronavirus. Last updated May 18, 2020; cited July 1, 2020.
6.Bonilla-Escobar FJ. Leadership and Health: The Scientific Journal's Mission of Spreading Science in Times of Pandemic. Int J Med Students. 2020 Jan-Apr;8 (1):9–10.
7.World Bank. Congo, Dem. Rep. Country Data. Available from: https://data.worldbank.org/country/congo-dem-rep?view=chart. Last updated October 20, 2019; cited July 1, 2020.
8.Komer L. COVID-19 amongst the Pandemic of Medical Student Mental Health. Int J Med Students. 2020 Apr 30;8 (1):56–7.
9.Kursumovic E, Lennane S, Cook T. Deaths in Healthcare Workers Due to COVID-19: The Need for Robust Data and Analysis. Anaesthesia. 2020 May 12; Epub 2020.
10.Siraj A, Khan MW. Uncertainty in the Air: In the Emergency Room with COVID-19 in Pakistan. Int J Med Students. 2020 Apr 30;8 (1):54–5.
Olga Djoutsop Mbougo, 1 Faculty of Medicine, Bel Campus University of Technology, Kinshasa, Democratic Republic of Congo
Vanessa Youmbi Nono, 1 Faculty of Medicine, Bel Campus University of Technology, Kinshasa, Democratic Republic of Congo
Ulrick S. Kanmounye, 1 Faculty of Medicine, Bel Campus University of Technology, Kinshasa, Democratic Republic of Congo
Francisco Javier Bonilla-Escobar, Editor
Lakshmimathy Subramanian, Student Editor
About the Author: Olga Djoutsop Mbougo is currently a seventh-year medical student at the Bel Campus University of Technology, Kinshasa, DRC of a 7-year program. She is also a recipient of the Dean's Award for academic excellence.
Correspondence: Olga Djoutsop Mbougo, Address: 17, 8ème Rue Limete / Quartier Industriel, Congo - Kinshasa Email: olgadjoutsop@gmail.com
Cite as: Djoutsop Mbougo O, Youmbi Nono V, Kanmounye US. COVID-19 and Clinical Rotations in the Democratic Republic of Congo. Int J Med Students. 2020 May-Aug;8(2):177-9.
Copyright © 2020 Olga Djoutsop Mbougo, Vanessa Youmbi Nono, Ulrick S. Kanmounye
This work is licensed under a Creative Commons Attribution 4.0 International License.
International Journal of Medical Students, VOLUME 8, NUMBER 2, August 2020