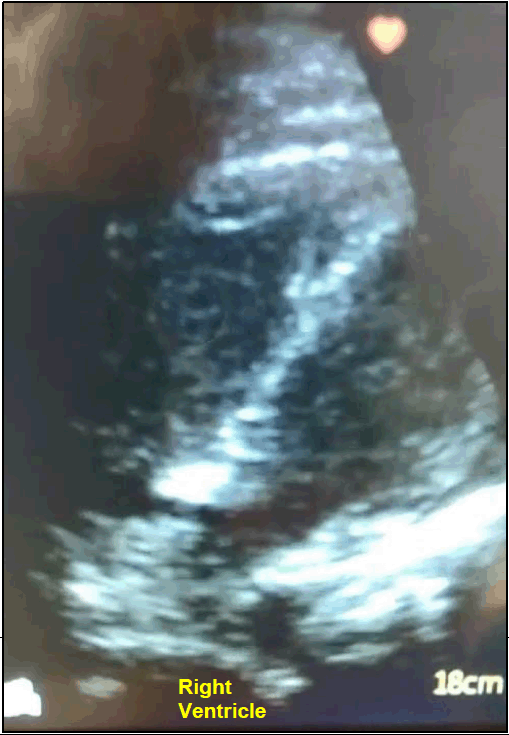
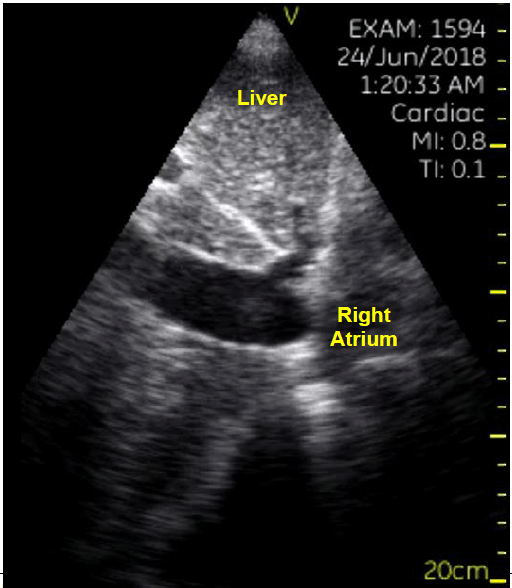
Subcostal view showing enlarged right ventricle (RV).
Re'em Sadeh1, Tomer Gat1, Omer Kaplan1, Tzvika Porges12, Lior Zeller13, Leonid Barski13, Lior Fuchs14
doi: http://dx.doi.org/10.5195/ijms.2021.558
Volume 9, Number 1: 15-20
Received 05 05 2020: Rev-request 24 11 2020: Rev-request 27 01 2021: Rev-recd 17 12 2020: Rev-recd 13 04 2021: Accepted 18 04 2021
ABSTRACT
Background:As point-of-care ultrasound (POCUS) becomes a standard of care procedure, medical schools around the world have started to seek the integration of POCUS courses into their curricula. This puts medical students in a unique position as they are trained in an area in which many physicians lack knowledge. This case series provides a glimpse into the capabilities of POCUS even when used by medical students.
Methods:Fourth-year medical students at Ben-Gurion University of the Negev performed numerous POCUS exams during their first clinical rotation at Soroka University Medical Center in Israel. All students completed a course in basic POCUS training and were evaluated in a brief practical exam before entering their first clinical rotation. Four of the cases in which the students took part are presented in this case series.
Results:The POCUS exam in the first case discovered pulmonary embolism in addition to the diagnosis of Cushing disease. In the second case, endocarditis could have been diagnosed three days earlier had a POCUS exam been performed. Case 3 demonstrates the additional contribution of POCUS to the decision-making process carried out by physicians and its superiority in quantifying and diagnosing pleural effusion compared to chest X-Ray. Case 4 indicated that POCUS is preferable over chest X-ray and auscultation for the diagnosis of pulmonary edema.
Conclusion:This case series may emphasize the capabilities POCUS has when utilized in the standard physical examination and the importance of incorporating POCUS instruction in medical schools for new physicians to acquire this skill.
Keywords: Point of Care Ultrasound; Internal medicine; Medical Education; Pulmonary embolism; Pulmonary edema (Source: MeSH-NLM).
Medical education is constantly challenged to keep up with the advances in medical technology.1 Point of care ultrasound (POCUS), a rapidly evolving area in medicine, has become an integral element of the physical examination, leading to its integration in medical schools' curricula.2
The advantages of POCUS have been demonstrated in numerous studies.3–7 Utilizing ultrasound at the bedside as a means of enhancing the physical examination by providing immediate clinical information, in turn aids the physician in building a diagnosis and assists in the clinical decision-making process. Previous data reports that POCUS can result in shorter time to diagnosis among dyspneic patients; reduced duration of mechanical ventilation; shortened length of stay in intensive care units; and expedited discharge time among heart failure patients when used in tailoring diuretics therapy.8–10 Additionally, POCUS exams are easily repeatable as the patients' condition evolves, providing rapid feedback as an evaluative tool in the treatment plan.
As POCUS is an operator-dependent modality, it is essential that the POCUS operator is highly skilled to correctly achieve the different ultrasound views and interpret them accurately. Hence, the concept of introducing POCUS training as early as during medical school is key. Indeed, medical schools around the world seek to integrate POCUS courses into their curricula.11,12 Many efforts are devoted to building POCUS training programs as well as evaluating which materials are fundamental for training. Dinh et al. defined milestones in training medical students to perform POCUS.13 A modified Delphi technique was used to identify milestones in the study of clinical ultrasound among fourth-year medical students. Out of 214 proposed milestones, 90 were chosen as the main milestones. Primarily in ultrasound physics and machine use were 27 milestones (30%), 13 milestones in cardiology (14.4%), 11 in thoracic (12.2%) and 6 milestones in abdominal ultrasound (6.7%).13 Another study developed a novel four-year-long vertical curriculum: During the first two years of medical school, students are taught basic ultrasound science and image acquisition.14 In the following two years, students are trained in ultrasound indications and interpretation.14,15
Ben-Gurion University of the Negev (BGU) has become invested in educating its medical students to perform POCUS at a sufficient level of expertise. As of 2017, each class takes an eight-hour-long POCUS course taught by senior intensive care unit (ICU) physicians and cardiologists. The purpose of the course is to integrate POCUS into the physician's daily practice and to teach how to improve the traditional physical examination utilizing the POCUS exam.16 Throughout the course, medical students are trained to perform ultrasound exams in echocardiography as well as focus assessment sonography in trauma (FAST) exams and lung ultrasound. The course is mandatory, and each class is comprised of 120 students who are later dispersed to clinical rotations in the internal medicine wards. In total, around 480 students underwent the POCUS course. The integration of POCUS into the Ben-Gurion medical school curriculum commenced in 2017, therefore the effects of this process on patient management and outcomes has yet to be studied in our institution. This POCUS course is unique in medical training in Israel. No other faculty in the country trains students to conduct a full cardiac POCUS examination.
As part of today's medical curricula, recently graduated physicians acquire POCUS skills that senior doctors may not possess, thus putting the former in a unique position. Senior medical staff might not be familiar with POCUS or have the awareness of the advantages this resource provides in early diagnosis and treatment. This situation creates fertile ground for recently graduated medical staff and students to provide significant added value in the clinical practice. A skilled POCUS operator can be a source of knowledge to the rest of the medical staff, despite a lack of vast clinical experience.
We have thus sought to describe certain cases where the use of POCUS augmented the physical examination and changed the primary patient diagnosis and management. The objective of this case series is to provide a glimpse into the capabilities of POCUS even when used by medical students.
This case series was initiated retrospectively by 3 fourth-year medical students at Ben-Gurion University in Be'er Sheva, Israel, who recorded their POCUS exams during their internal medicine rotation. The rotation took place over three months, during clinical rotations in an internal medicine ward, between March and June of 2018. All students underwent a cardiac POCUS course prior to the rotation.
All fourth-year medical students from the BGU six-year-long medical school program receive POCUS training before arriving at their first clinical rotation. The training focuses mainly on the principle of transthoracic echocardiographic views providing the capability to perform and analyze all basic cardiac ultrasound views.
Training includes:
Students practiced on cardiac and lung simulators and on their colleagues using pocket and cardiovascular ultrasound devices (Simbionix Simulator, Vscan and Vivid S70 GE Healthcare). At the end of the 10-hour course students' proficiency was evaluated based on a 6-minute views test described elsewhere.16
During the fourth year of a six-year medical school program, all students rotate through internal medicine for three months. This is their first clinical rotation and was taken in various wards at Soroka University Medical Center (SUMC), a large tertiary medical center in Israel's southern region. Among their rotation obligations, students are required to take part in rounds, obtain medical history, perform physical examinations and write admission notes on patients admitted to the internal medicine ward from the emergency department, all under the supervision of an internal medicine attending physician or resident. Most student-patient interactions took place after the patient was already examined by the primary team and the first diagnostic and treatment plan was established.
Students were encouraged to incorporate POCUS in their first patient assessment as part of the physical examination. After the students completed the admission process, they were required to present their patients to the medical resident taking care of the patient as well as presenting the POCUS findings to ultrasound experts at the time of the examination or via recorded video of the examination, when available. The ultrasound device used in the cases presented in this study was a Vscan-GE healthcare. In most internal medicine wards, physicians were not trained in POCUS, a skill which the students, who underwent a professional POCUS course recently introduced at BGU medical school, had acquired. The physicians presented in this study did not go through similar training.
All participants signed an informed consent form approving the information written in this manuscript.
In this case series, we will present four cases in which medical students contributed to the assessment and treatment of their patients by adding important clinical findings as a direct result of POCUS (Table 1).
Table 1.Patients' presentations and POCUS findings.
| Case | Presentation/Preliminary Diagnosis | Student POCUS finding* | Pt new diagnosis | Management Change |
|---|---|---|---|---|
| 1 | Effort dyspnea, presumed secondary to Cushing's Syndrome | Enlargement of right ventricle Right ventricle hypokinesis | Bilateral PE | Prompt CTA exam was ordered followed by anticoagulation treatment. |
| 2 | Fever of unknown origin (FUO) | Vegetation on mitral valve | Mitral valve endocarditis was identified 4 days before formal TTE | Proper endocarditis antibiotic treatment was started 4 days earlier rather than empiric antibiotic treatment for FUO |
| 3 | Dyspnea, presumed to be secondary to large pleural effusion | Lung ultrasound revealed only small amount of pleural effusion and ultrasonographic signs of pulmonary congestion | Pulmonarycongestion | Thoracentesis was deferred and diuretics for lung congestion were initiated |
| 4 | Dyspnea of unknown cause | Multiple bilateral B lines and no imaging of lung consolidation | Pulmonary edema | Initiation of Furosemide treatment |
A 40-year-old female with a medical history of hypertension was admitted one month before the current admission with shortness of breath, hirsutism, and amenorrhea. The patient had a work-up for Cushing Syndrome and high 24-hour urine cortisol levels were detected. She was readmitted due to effort dyspnea and dizziness, presumably unrelated to the diagnosis of Cushing Disease which was defined as her primary diagnosis. During the current admission additional tests were ordered, including a head CT and chest X-ray (CXR). Ophthalmology and neurology evaluations were ordered as well.
She was examined by a fourth-year student during their first clinical rotation. The student performed a physical examination revealing bilateral leg edema with no erythema, tenderness or palpable chords and no findings in heart and lung auscultation. Vital signs were normal except for high blood pressure. In addition, the student performed a POCUS study revealing significant global right ventricular (RV) hypokinesis and enlargement that was not known to the primary team. (Figure 1). Furthermore, the left ventricle (LV): RV ratio was reversed (RV bigger than the LV). The medical team was notified by the student; the POCUS findings, concomitant leg edema, and relative immobilization raised the concern for a pulmonary embolism. A pulmonary CT angiography test was ordered, revealing significant bilateral pulmonary embolisms. Appropriate treatment was initiated. Three days later, the patient improved significantly and was discharged from the medical center.
Figure 1.Subcostal view showing enlarged right ventricle (RV).

A 19-year-old female with no previous medical history was admitted to the internal medicine ward with persistent fever for two weeks reaching 40 degrees Celsius, which was treated with antipyretics. On her physical examination, the patient seemed lethargic with the only major clinical finding being a systolic murmur 3/6 radiating to the mid-axillary area. A transthoracic echo (TTE) was ordered (scheduled for a future date) and empiric antibiotic therapy with ceftriaxone was initiated due to fever of unknown origin.
A fourth-year medical student in their first clinical rotation, performed a physical examination augmented by POCUS study on the patient's first day of admission. The student identified a small mobile mass on the mitral valve using POCUS. The primary team was notified, multiple blood cultures were taken, and proper endocarditis antibiotic therapy was initiated.
Due to technical reasons, only on the fourth day of admission was the formal TTE study conducted. At this point in time, the patient was formally diagnosed with endocarditis and continued the previously subscribed systemic endocarditis antibiotic therapy.
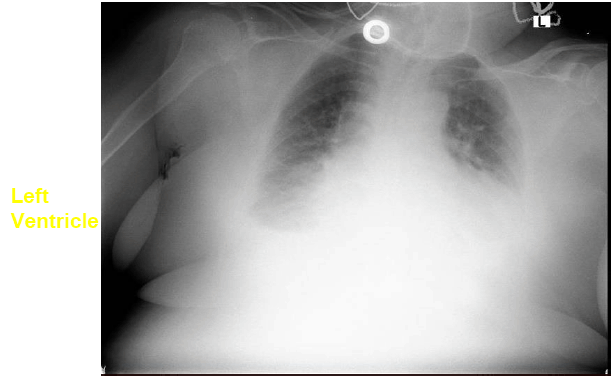
An 84-year-old female with a medical history of congestive heart failure (CHF) and uncontrolled hypertension was admitted due to dyspnea and productive cough which started three days prior to her admission. Decreased breathing sounds were auscultated over the left lower lung. AP chest X-ray was interpreted as consistent with a large volume left sided pleural effusion (Figure 2). The patient's diagnosis was CHF exacerbation due to uncontrolled hypertension. In addition to the standard treatment for CHF exacerbation, the medical team deduced that the significant pleural effusion found on the chest X-ray contributed to the patient's dyspnea and therefore was scheduled for non-image-guided left side thoracentesis.
Figure 2.Chest X-ray showing significant left-sided effusion concealing the cardiac silhouette, and blunting of the right costophrenic angle suggesting a small right-sided effusion.
A fourth-year medical student, in his first clinical rotation, performed a physical examination augmented by POCUS study. The student's examination contradicted the chest X-ray, finding only a small amount of pleural effusion which is presented as a small restricted black area (representing fluid) above the diaphragm. Findings were reported to the primary team. This finding was later verified by an internist with POCUS experience. Due to the student's findings, thoracentesis was cancelled. Treatment with diuretics was initiated and the patient improved significantly.
In this case, an unnecessary invasive action was prevented due to the presence of an ultrasound operator. The chest X-ray evaluation suggested a large left-sided pleural effusion. Even though chest X-rays are notoriously inaccurate in evaluating the volume of pleural effusions they are sometimes used due to the lack of more specific techniques. However, the presence of a fourth-year medical student with basic POCUS skills presented an alternative option and gave a more accurate reading of a small pleural effusion, which did not require a thoracentesis.
An 86-year-old male with hypertension was admitted to the emergency room (ER) with a chief complaint of dyspnea at rest that started the previous evening. The patient was tachycardic (heart rate was approximately 100 beats per minute) and tachypneic (respiratory rate of 24 breaths per minute) with a temperature of 37.8 degrees Celsius. Chest X-ray taken in the emergency ward was inconclusive, showing mild infiltrates on the bases of both lungs. The patient was admitted to the internal medicine ward for further evaluation and treatment.
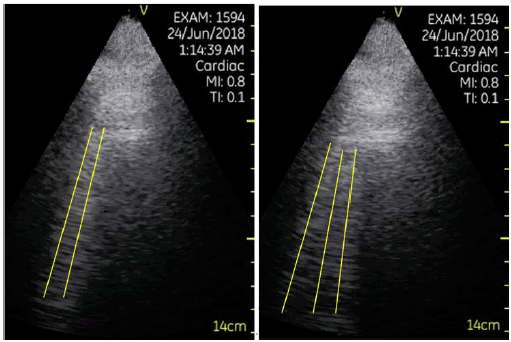
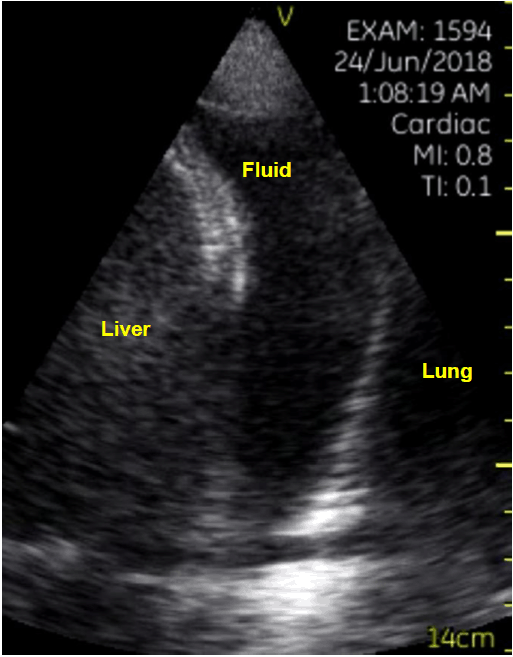
On day one of admission, neither history taking nor physical examination, conducted by the resident, clarified the diagnosis or reason for dyspnea. The patient was known to suffer from hypertension, tobacco use, lack of exercise and had no recent contact with sick people. The physical examination did not show jugular vein distention or peripheral edema; however, on auscultation soft crackles were heard. Hence, along with sub-febrile temperature, new dyspnea and the presented information, the possibility of pneumonia and pulmonary congestion secondary to heart failure was listed in the differential diagnosis. At this point, a lung POCUS exam was performed by a fourth-year medical student in their first clinical rotation as part of the physical examination of the patient. The student found multiple ultrasonographic B lines (Figure 3), pleural effusions (Figure 4) in the bases of both lungs, and a non-collapsible IVC (Figure 5). No lung hepatization or dynamic air bronchograms were present. Therefore, combining data from the chest X-ray and POCUS of the lungs, lung consolidation was ruled out and lung edema was diagnosed. The primary team initiated furosemide treatment based on the lung POCUS findings and the patient improved significantly. Further investigations suggested that the pulmonary edema was a result of poor compliance to his hypertension and heart failure treatment.
Figure 3.Mid-axillary view of the base of the lungs demonstrates three B-Lines and more.
Fluid between the pleural membranes.
Non-collapsible inferior vena cava (IVC).
In this study we presented four cases in which medical students with basic POCUS skills were able to change the primary diagnosis as well as the treatment plan of newly admitted patients in internal medicine wards. Physicians use multiple resources to promote a timely diagnosis and appropriate treatment. Lacking knowledge in POCUS deprives both the physician and the patient of a valuable diagnostic tool for patient evaluation and appropriate treatment.
We practice medicine in a transitional time where POCUS has entered the curriculum of some medical schools, but many senior and experienced physicians do not hold this new bedside capability. This creates a reality where medical students can use ultrasound to ‘see into their patients' when other physicians may only be comfortable to auscultate, palpate or percuss.10,17
In all four cases, patients received thorough assessment by a number of senior physicians prior to the students POCUS exam. However, the traditional clinical tools used by the physicians did not suffice, and the final diagnosis of the condition was reached through a POCUS examination conducted by one of the students. The POCUS examination conducted by the students produced critical information that reduced the time to correct diagnosis and changed the course of treatment.
It is worth mentioning that the clinical role of POCUS is not to make a definitive diagnosis. POCUS is meant to accelerate the process of diagnosis and treatment and assist in the decision-making process.18,19 As seen in the cases presented, POCUS examination conducted by the students led to faster diagnosis and treatment. When necessary, the POCUS examination was followed by a definitive gold standard test which confirmed the findings found on the POCUS examination.
In case 1, performing a POCUS exam during the patient's first dyspnea admission, one month earlier, would probably have led to an earlier discovery of the PE, a life-threatening disease, thus saving the patient from a month of symptoms, another admission and potentially her life.
Case 2 is an example of how POCUS might provide information leading to the proper diagnosis and appropriate antibiotic treatment three days earlier. In this case of fever of unknown origin versus final diagnosis of endocarditis, time to proper antibiotic therapy may have been crucial. Ideally, the patient should have received diagnostic transthoracic echocardiography immediately after the cardiac murmur was discovered; but in the real medical world, days can often elapse from admission to the proper diagnostic study.
Case 3 is an example of how a POCUS exam contributed to the physicians' confidence in their decision-making process. An additional, objective observation is sometimes critical and may spare harmful procedures.
In Case 4, the POCUS exam had a significant effect on the course of treatment and demonstrated superiority over chest X-ray and auscultation for the diagnosis of pulmonary edema. In 2004, Liechtenstein D. et al compared auscultation, chest X-ray and lung ultrasound in acute respiratory distress syndrome (the most acute form of pulmonary edema) and showed far better sensitivity with lung ultrasound compared to chest X-ray and auscultation (93%, 68% and 8% respectively).20 Ten years later, Al Deeb et al showed in their meta-analysis that the sensitivity and specificity of POCUS using B-lines to diagnose pulmonary edema is 94.1% and 92.4% respectively.21 In the presented case, the primary team could not determine whether the dyspnea was a result of pulmonary congestion or pneumonia, and without the availability of a POCUS exam the patient would probably have gone through many more tests and exams, delaying symptomatic relief.
The concept of ‘ultrasound stethoscope' is rapidly moving from theory to reality.11,22 Our fourth-year students, having better training in POCUS over the more senior in-house physicians and residents with no POCUS experience at all were able to significantly alter the diagnosis and improve the treatment of their patients. There are many difficulties in the process of teaching POCUS to medical students: it is an operator-dependent modality necessitating small-group bedside teaching, it is sometimes opposed by senior traditional medical staff, condensed medical school curriculums, lack of available POCUS experts, lack of mobile ultrasound machines and more. However, like other recent studies, this case series demonstrates the importance of developing medical schools' curriculum in this field.23,24
Garnier et al. presents an example of the impact POCUS courses have when incorporated in medical schools, describing the impact of a pilot emergency medicine ultrasonography course on medical students' knowledge.25 They demonstrated a significant improvement in ultrasound knowledge improving the total score in an ultrasound questionnaire test from 59.7% correct answers before the course to 86% after. In addition, after the course 96.5% of participants were able to complete an extended FAST scan. Other medical schools should also adopt and develop novice tools to teach students the art of the new augmented bedside physical examination. To overcome the difficulties of teaching POCUS and minimize the disadvantage of this modality as an operator-dependent skill, we believe students at the beginning of their POCUS experience should be accompanied by POCUS mentors, with whom they may discuss specific cases and can consult regarding different findings, so that the right conclusions will be made and to avoid misdiagnoses. We think courses should start early in medical education, in anatomy classes the ultrasound can facilitate an understanding of topographic anatomy, while incorporating, for example, cardiac ultrasound anatomy sessions.26 In addition, cardiac ultrasound courses should be incorporated in physical examination classes and shock cases. Nevertheless, there are many setbacks preventing POCUS from becoming an inherent part of modern medicine worldwide; POCUS training is extremely time consuming and requires many resources as compared with other subjects taught in medical schools. Since POCUS is a manual skill, hands-on training must be taught in small groups; this requires proper facilities, paid models to simulate patients, ultrasound devices, and tutors who are usually physicians or senior students. Ohio State University College of Medicine reports major challenges in funding POCUS training due to the high cost of ultrasound machines and difficulties integrating the new curricula into existing teaching methodologies. 14 The University of South Carolina integrated an ultrasound curriculum taught throughout four years of medical school, and reported similar difficulties in terms of faculty experience, administrative and clinical specialty support, and available resources.15
In order to overcome these difficulties in our faculty, we train students to teach and train other students in POCUS, saving money and time from senior physicians teaching hours. Web-based applications are trying to be used for POCUS self-learning.16 Our faculty purchased a number of second-hand ultrasound machines and a simulator which can simulate many different clinical pathologies and clinical scenarios enabling students to practice on their own time.
Comprehensive POCUS training will contribute to our next generation of physicians, significantly improving their bedside diagnostic capabilities, shortening time to definitive treatment, and improving overall patient care.9–11
This study took place before the COVID-19 outbreak. However, it is worth noting that in addition to the everyday advantages of POCUS such as being an accessible and easy-to-operate tool that does not expose patients to radiation, POCUS is also valuable when considering its low risk of infection. POCUS may reduce the exposure and risk of infection in comparison to a CT scan or a chest X-ray, in which the patient is required to move around the hospital or be exposed to machines which can be difficult to disinfect.27
As this study is a case series, the main limitations of this study include the small sample size and retrospective, not longitudinal data collection. This limits our understanding of the impact of medical students trained in POCUS.
Medical students in their first clinical rotation were able to change diagnoses of four internal medicine ward patients when incorporating POCUS to the traditional physical examination. Their findings altered medical therapy and management. There is a knowledge gap between medical students receiving POCUS training and more senior physicians who have not received training in POCUS. Efforts should be made to close this gap and to further incorporate POCUS teaching in medical schools as well as for more senior physicians.
None.
The Authors have no funding, financial relationships or conflicts of interest to disclose.
Conceptualization: RS, LF. Investigation: RS, TG, OK. Methodology: LF. Supervision: TP, LZ, LB, LF. Validation: TP, LZ, LB, LF. Visualization: RS, TG, OK. Writing – Original Draft: RS. Writing – Review & Editing: TP, LZ, LB, LF.
1. Harden RM. Ten key features of the future medical school—not an impossible dream. Med Teach. 2018 Oct;40(10):1010–1015.
2. Kobal SL, Lior Y, Ben-Sasson A, Liel-Cohen N, Galante O, Fuchs L. The feasibility and efficacy of implementing a focused cardiac ultrasound course into a medical school curriculum. BMC Med Educ. 2017 May;17(1):1–9.
3. Labovitz AJ, Noble VE, Bierig M, Goldstein SA, Jones R, Kort S, et al. Focused cardiac ultrasound in the emergent setting: A consensus statement of the American society of Echocardiography and American College of Emergency Physicians. J Am Soc Echocardiogr. 2010 Dec;23(12):1225–30.
4. Cortellaro F, Colombo S, Coen D, Duca PG. Lung ultrasound is an accurate diagnostic tool for the diagnosis of pneumonia in the emergency department. Emerg Med J. 2012 Jan;29(1):19–23.
5. Reissig A, Copetti R, Mathis G, Mempel C, Schuler A, Zechner P, et al. Lung ultrasound in the diagnosis and follow-up of community-acquired pneumonia: A prospective, multicenter, diagnostic accuracy study. Chest. 2012 Oct;142(4):965–72.
6. Zanobetti M, Poggioni C, Pini R. Can chest ultrasonography replace standard chest radiography for evaluation of acute dyspnea in the ED? Chest. 2011 May;139(5):1140–7.
7. Zanobetti M, Scorpiniti M, Gigli C, Nazerian P, Vanni S, Innocenti F, et al. Point-of-Care Ultrasonography for Evaluation of Acute Dyspnea in the ED. Chest. 2017 Jun;151(6):1295–301.
8. Girard M, Migner-Laurin G. Time for a New Consensus on Lung Ultrasonography. Chest. 2016 Oct;150(4):986–7.
9. Chen Z, Hong Y, Dai J, Xing L. Incorporation of point-of-care ultrasound into morning round is associated with improvement in clinical outcomes in critically ill patients with sepsis. J Clin Anesth. 2018 Aug;48(3):62–6.
10. Mozzini C, Di Dio Perna M, Pesce G, Garbin U, Fratta Pasini AM, Ticinesi A, et al. Lung ultrasound in internal medicine efficiently drives the management of patients with heart failure and speeds up the discharge time. Intern Emerg Med. 2018 Jan;13(1):27–33.
11. Solomon SD, Saldana F. Point-of-Care Ultrasound in Medical Education — Stop Listening and Look. N Engl J Med. 2014 Mar;370(12):1083–5.
12. Rao S, Van Holsbeeck L, Musial JL, Parker A, Bouffard JA, Bridge P, et al. A pilot study of comprehensive ultrasound education at the Wayne State University School of Medicine: A pioneer year review. J Ultrasound Med. 2008 May;27(5):745–9.
13. Dinh VA, Lakoff D, Hess J, Bahner DP, Hoppmann R, Blaivas M, et al. Medical student core clinical ultrasound milestones: A consensus among directors in the United States. J Ultrasound Med. 2016 Feb;35(2):421–34.
14. Bahner DP, Adkins EJ, Hughes D, Barrie M, Boulger CT, Royall NA. Integrated medical school ultrasound: Development of an ultrasound vertical curriculum. Crit Ultrasound J. 2013 Jul 2;5(1):6.
15. Hoppmann RA, Rao V V., Poston MB, Howe DB, Hunt PS, Fowler SD, et al. An integrated ultrasound curriculum (iUSC) for medical students: 4-year experience. Crit Ultrasound J. 2011 Apr;3(1):1–12.
16. Fuchs L, Gilad D, Mizrakli Y, Sadeh R, Galante O, Kobal S. Self-learning of point-of-care cardiac ultrasound - Can medical students teach themselves? PLoS One. 2018 Sep;13(9):1–12.
17. Narula J, Chandrashekhar Y, Braunwald E. Time to add a fifth pillar to bedside physical examination inspection, palpation, percussion, auscultation, and insonation. JAMA Cardiol. 2018 Apr;3(4):346–50.
18. Smith D, Walters EL, Reibling E, Brockie D, Lee C, Neeki M, et al. Unified: Understanding new information from emergency departments involved in the San Bernardino terrorist attack. West J Emerg Med. 2020 Feb;21(2):382–90.
19. Kovell LC, Ali MT, Hays AG, Metkus TS, Madrazo JA, Corretti MC, et al. Defining the Role of Point-of-Care Ultrasound in Cardiovascular Disease. Am J Cardiol. 2018 Oct;122(8):1443–50.
20. Lichtenstein D, Goldstein I, Mourgeon E, Cluzel P, Grenier P, Rouby JJ. Comparative Diagnostic Performances of Auscultation, Chest Radiography, and Lung Ultrasonography in Acute Respiratory Distress Syndrome. Anesthesiology. 2004 Jan;100(1):9–15.
21. Al Deeb M, Barbic S, Featherstone R, Dankoff J, Barbic D. Point-of-care ultrasonography for the diagnosis of acute cardiogenic pulmonary edema in patients presenting with acute dyspnea: A systematic review and meta-analysis. Acad Emerg Med. 2014 Aug;21(8):843–52.
22. Moore CL, Copel JA. Point-of-care ultrasonography. N Engl J Med. 2011 Feb; 364(8):749–57.
23. Alber KF, Dachsel M, Gilmore A, Lawrenson P, Matsa R, Smallwood N, et al. Curriculum mapping for focused acute medicine ultrasound (FAMUS). Acute Med. 2018;17(3):168.
24. Watson K, Lam A, Arishenkoff S, Halman S, Gibson NE, Yu J, et al. Point of care ultrasound training for internal medicine: A Canadian multi-centre learner needs assessment study. BMC Med Educ. 2018 Sep;18(1):1–8.
25. Wisniewski J, Garnier H. Lifesaving Sonography Protocols: A Pilot Course Involving Undergraduate Medical Students. Int J Med Students. 2015 Mar;3(1):15–8.
26. Garnier H, Plosaj P, Wisniewski J. Ultrasonography as a Modern Teaching Support to the Anatomy Course: Is It Beneficial for Medical Students. Int J Med Students. 2015 Jun;3(2):119.
27. Yasukawa K, Minami T. Point-of-care lung ultrasound findings in patients with COVID-19 Pneumonia. Am J Trop Med Hyg. 2020 Jun;102(6):1198–202.
Re'em Sadeh, 1 Medical student, Joyce and Irwing Goldman Medical School, Ben-Gurion University of the Negev, Beer-Sheva, Israel
Tomer Gat, 1 Medical student, Joyce and Irwing Goldman Medical School, Ben-Gurion University of the Negev, Beer-Sheva, Israel
Omer Kaplan, 1 Medical student, Joyce and Irwing Goldman Medical School, Ben-Gurion University of the Negev, Beer-Sheva, Israel
Tzvika Porges, 1 Medical student, Joyce and Irwing Goldman Medical School, Ben-Gurion University of the Negev, Beer-Sheva, Israel
2 MD, Medical internal Ward Internal Medicine B, Soroka University Medical Center and The Faculty of Health Sciences, Ben-Gurion University of the Negev, Beer-Sheva, Israel
Lior Zeller, 1 Medical student, Joyce and Irwing Goldman Medical School, Ben-Gurion University of the Negev, Beer-Sheva, Israel
3 MD, Internal Medicine F, Soroka University Medical Center and The Faculty of Health Sciences, Ben-Gurion University of the Negev, Beer-Sheva, Israel
Leonid Barski, 1 Medical student, Joyce and Irwing Goldman Medical School, Ben-Gurion University of the Negev, Beer-Sheva, Israel
3 MD, Internal Medicine F, Soroka University Medical Center and The Faculty of Health Sciences, Ben-Gurion University of the Negev, Beer-Sheva, Israel
Lior Fuchs, 1 Medical student, Joyce and Irwing Goldman Medical School, Ben-Gurion University of the Negev, Beer-Sheva, Israel
4 MD, Medical Intensive Care Unit, Soroka University Medical Center and The Faculty of Health Sciences, Ben-Gurion University of the Negev, Beer-Sheva, Israel
About the Author: Re'em is currently a sixth-year medical student and a senior ultrasound instructor. With the COVID-19 pandemic spreading throughout the world, he has been training physicians all around the country in lung ultrasound, an invaluable technique in the management of COVID-19 patients.
Correspondence: Re'em Sadeh, Address: Caroline House, Faculty of Health Sciences, Ben-Gurion University of the Negev Be'er Sheva, 8410501, Israel. Email: reem.sadeh90@gmail.com
Editor: Shawn Albers, Francisco J. Bonilla-Escobar Student Editor: Vivek Podder Copyeditor: Adam Dinoff Proofreader: Madeleine Jemima Cox Layout Editor: Annora Ai-Wei Kumar
Copyright © 2021 Re'em Sadeh, Tomer Gat, Omer Kaplan, Tzvika Porges, Lior Zeller, Leonid Barski, Lior Fuchs
This work is licensed under a Creative Commons Attribution 4.0 International License.
International Journal of Medical Students, VOLUME 9, NUMBER 1, April 2021