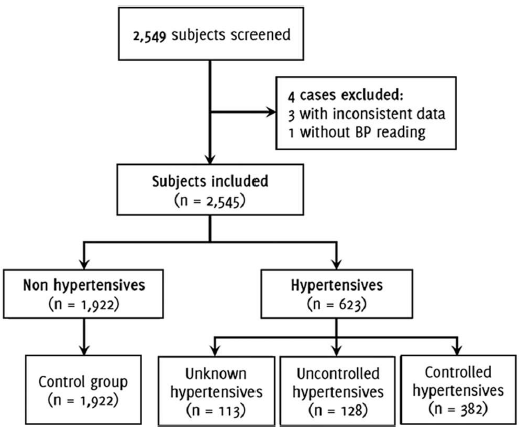
Study Flowchart.
José Adrián Yamamoto-Moreno1, Suzzette Anaís Navarro-Rodríguez2, Samuel Ruiz-Pérez3, Juan Carlos Godínez-Reyes4, Marvin Mendoza-Rojo5
doi: http://dx.doi.org/10.5195/ijms.2020.639
Volume 8, Number 3: 263-272
Received 01 09 2020: Rev-request 29 09 2020: Rev-request 28 10 2020: Rev-recd 30 09 2020: Rev-recd 30 11 2020: Accepted 01 12 2020
ABSTRACT
Background:Hypertension remains a growing public health concern in Mexico. This study aims to describe hypertension awareness, treatment, control, and its associated factors in participants of an opportunistic, medical student-led blood pressure screening campaign in Mexico.
Methods:A cross-sectional study using convenience sampling was performed, including participants aged 18 years and older from 15 Mexican states. Each participant completed a questionnaire about risk factors and had three blood pressure measurements taken. Hypertension was defined as ≥140/90 mmHg. Multiple imputation with linear regression was performed where data was missing.
Results:From a population of 2,545 participants, 623 (24.5%) participants had hypertension. Of those with hypertension, 81.9% had a previous diagnosis of hypertension, and only 16.1% were not on medication at the time of screening; 61% were controlled, 21% were uncontrolled patients, and 18% were not aware they had hypertension. The largest proportion of uncontrolled cases (33%) were found in states with high marginalization, and the number of unaware hypertensives in very low marginalization states were double that of the national figure. More than half of the participants taking antihypertensive agents were on a single medication, achieving control in almost 8 in 10 patients.
Conclusion:Most uncontrolled hypertensive patients in Mexico belong to marginalized states. These results could inform state legislative policy to help bridge healthcare gaps.
Keywords: Hypertension; Blood Pressure; Screening; Mexico (Source: MeSH-NLM).
Hypertension is a chronic, controllable disease of multifactorial etiology, characterized by a sustained increase in blood pressure (BP) levels.1 Its importance lies in the fact that it is the most common risk factor for the development of cardiovascular disease (CVD), which is the leading cause of death worldwide, generating approximately 10.5 million deaths per year.2,3
In high-income countries, an improvement in the awareness, treatment, and control of the disease has been observed.4 Healthcare systems in countries with better control of hypertension such as the United States, Canada, South Korea, and Germany all have health education or health check-up programs.5 However, in low and middle-income countries such as Brazil, China, India, Indonesia, Mexico, and South Africa, the results of disease prevention strategies have been less favorable, revealing a need to improve health services and prevention programs.6
In Latin America, 40% of the adult population suffers from hypertension. This can be attributed to considerable variations in hypertension awareness, treatment and control depending on race/ethnicity, sex, income, occupation, education, social position, psychosocial and behavioral factors, among other social aspects.7 For example, people with a higher socioeconomic level are more likely to be physically inactive, with physical inactivity being one of the main risk factors for hypertension.7 On the other hand, better adherence to treatment has been observed in people with a higher educational level.8 Small studies have shown that the majority of people living with hypertension do not know the normal BP levels and that there is a correlation between body weight and elevated BP.9
Hypertension is still a growing public health concern in Mexico. The National Health and Nutrition Survey (ENSANUT) reported prevalence figures of 25.5%, of which 40.0% were not aware they had hypertension. Among those who were previously diagnosed with hypertension, 79.3% received pharmacological treatment, and only 45.6% were properly controlled.10 An estimated increase of 151% is expected in the number of individuals needing care for hypertension by 2050 if further actions are not taken in Mexico.8
Several global campaigns have been devised to improve awareness and early detection of hypertension—such as the May Measurement Month (MMM)—a global screening intervention performed on an annual basis by the International Society of Hypertension (ISH). This campaign focuses on measuring BP among the general population and identifying risk and predisposing factors for the disease.3,6 The 2019 intervention had a response from more than 100 countries, with a final count of 1,508,130 participants worldwide.6
As an approach to addressing such problems in Mexico, the Asociación Mexicana de Médicos en Formación (AMMEF, the Mexican Association of Physicians in Training) took the initiative to perform an opportunistic BP screening campaign inspired by the MMM methodology.3,6 The aim of this study was to describe hypertension awareness, treatment, control, and its associated factors in participants of an opportunistic medical student-led BP screening campaign in Mexico.
This was a cross-sectional study using convenience sampling. A detailed protocol was developed to be used for all entities in the country. The full protocol can be consulted at http://ijms.info/IJMS/article/view/639/Supplementary_Material. The eligibility criteria for participants were an age of 18 years and older, and consent to participate in the study according to local policies. Online and face-to-face training was provided for leaders of local screening teams distributed in 15 states of Mexico about the questionnaire application and standardized methodology for BP measurements. The screening was performed in Aguascalientes, Baja California, Chihuahua, Chiapas, Coahuila, Durango, Guanajuato, México, Nayarit, Nuevo León, Puebla, San Luis Potosí, Sonora, Veracruz and Zacatecas. Sites of screening were set up in hospital waiting rooms, public outdoor or indoor areas, nursing homes, schools, homes, and workplaces.
Data were collected from the beginning of June to the end of October 2019 by volunteer medical students using an automated electronic device or an aneroid sphygmomanometer with a stethoscope. Recommendations for the measurement of BP included three seated recordings taken on the left (preferably) or right arm with a one-minute gap between readings.
The MMM questionnaire was created by the International Society of Hypertension (ISH); it consisted of 24 items with sociodemographic data; identification of risk factors; anthropometric and blood pressure measurements (https://maymeasure.com/get-involved/downloadable-resources).
Hypertension was defined as a systolic blood pressure (SBP) ≥140 mmHg or a diastolic blood pressure (DBP) ≥90 mmHg in at least two of the readings. Cases were classified as “unaware hypertensive” (UAH) patients for those that satisfy the hypertension definition at screening but did not have a previous diagnosis or treatment; “controlled hypertensive” (CH) population for those with normal BP values at screening but with a previous diagnosis or treatment for hypertension; “uncontrolled hypertensive” (UCH) patients were those that complied hypertension criteria at screening and had a diagnosis and/or treatment for hypertension; “non-hypertensive” (NH) population were those that did not satisfy any of the previous conditions. A control group was established, including participants without hypertension who declared taking no medication or having clinical signs of diabetes, with no history of stroke, myocardial infarction (MI), gestational hypertension (GH), pregnancy at the time of screening, smoking, and alcohol drinking. Associated factors to changes in BP were considered to be fasting, history of stroke, history of MI, diabetes, pregnancy, history of GH, tobacco smoking, alcohol consumption, body mass index (BMI) and heart rate. Screening locations were classified according to Social Gap Index (SGI) emitted by the National Council for the Evaluation of Social Development Policy, which ranks federal entities on five levels based on access to education, health, basic services and housing, from lowest to highest level of social inequality.11
According to the SGI, marginalization is very low in Aguascalientes, Coahuila and Nuevo León; low in Baja California, Chihuahua, State of Mexico, Sonora and Zacatecas; middle in Durango, Guanajuato and Nayarit; high in Puebla and San Luis Potosí and very high in Chiapas and Veracruz.11
Multiple imputation with linear regression was performed five times using the missing at random (MAR) assumption where data was missing for variables such as height, weight, and subsequent BP readings. Geographical localization, sex, medical history, SBP, and DBP measurements were used as indicators for multiple imputation. Missing values were replaced with the pooled imputed data, and the resulting dataset was tested for normality using the Kolmogorov-Smirnov test in a Monte Carlo simulation of 500 cases. For the analysis of attributable factors to changes in BP, mean SBP, and DBP of the control group were calculated, and used as reference All statistical analysis was performed using IBM SPSS Statistics for Windows (Armonk, NY) and began in June 2020.
From a total of 2,549 entries, the study included 2,545 participants after eliminating 4 entries as shown in Figure 1. Missing data was observed in 48 (1.80%) cases for height, 52 (2.04%) for weight, 800 (31.43%) for second BP reading, and 1,320 (51.47%) for third BP reading. An estimated error <2% in data distribution was observed after multiple imputation.
Figure 1Study Flowchart.

Roughly half of the screenings were carried out in open public areas (53.8%), followed by hospitals and clinics (26.8%), closed public areas (12.5%), homes (5.1%), workplaces (1.0%), educational institutions (0.5%) and nursing homes (0.3%). From the total number of participants included, 53.6% were women (see Table 1). Mean age was 41 years with a range from 18 to 91 years, with most participants in the 18 to 39 years age group, accounting for 50.6% of screened subjects. Almost a quarter (24.1%) of participants had a history of smoking, 57.7%declared having never or almost never consumed alcohol, 26.6% consumed alcohol between one and three times per month, and 15.3% at least once a week. Regarding diabetes, 6.9% of participants did not know if they had diabetes, whereas 11.4% declared having the diagnosis. Only 1.5% and 2.7% of participants had a history of stroke or MI, respectively. A history of GH was declared by 9.2% of women involved, and only 40 (1.6%) participants were pregnant at the time of screening.
Table 1.Demographic Characteristics of Participants.
| Variables | Hypertensive patients n = 623 (24.5%) | Non-hypertensive patients n = 1,922 (75.5%) | Total n = 2,545 |
|---|---|---|---|
| Sex, n (%) | |||
| Male | 303 (48.6%) | 878 (45.7%) | 1,181 (46.4%) |
| Female | 320 (51.4%) | 1,044 (54.3%) | 1,364 (53.6%) |
| Age, years (standard deviation) | |||
| Mean | 56 (15) | 36 (16) | 41 (73) |
| Range | 18–90 | 18–91 | 18–91 |
| Age group, n (%) | |||
| 18 to 39 years | 94 (15.1%) | 1,195 (62.2%) | 1,289 (50.6%) |
| 40 to 59 years | 262 (42.1%) | 531 (27.6%) | 793 (31.2%) |
| ≥60 years | 267 (42.9%) | 196 (10.2%) | 463 (18.2%) |
| History of diabetes, n (%) | |||
| Yes | 173 (27.8%) | 117 (6.1%) | 290 (11.4%) |
| No | 399 (64%) | 1,674 (87.1%) | 2,073 (81.5%) |
| Does not know | 51 (8.2%) | 131 (6.9%) | 133 (6.9%) |
| History of smoking, n (%) | |||
| Yes | 163 (26.3%) | 447 (23.4%) | 610 (24.1%) |
| No | 456 (73.7%) | 1,460 (76.6%) | 1,916 (75.9%) |
| Alcohol consumption, n (%) | |||
| 1 to 3 times per month | 132 (21.2%) | 546 (28.4%) | 678 (26.6%) |
| At least once a week | 89 (14.3%) | 301 (15.7%) | 390 (15.3%) |
| Never | 401 (64.4%) | 1,067 (55.5%) | 1,468 (57.7%) |
| Not declared | 1 (0.2%) | 8 (0.4%) | 9 (0.4%) |
| History of stroke, n (%) | |||
| Yes | 31 (5.1%) | 6 (0.3%) | 37 (1.5%) |
| No | 571 (94.9%) | 1,886 (99.7%) | 2,457 (98.5%) |
| History of myocardial infarction, n (%) | |||
| Yes | 55 (9.2%) | 13 (0.7%) | 68 (2.7%) |
| No | 543 (90.8%) | 1,884 (99.3%) | 2,427 (97.3%) |
| History of gestational pregnancy, n (%) | |||
| Yes | 73 (21.8%) | 65 (5.6%) | 138 (9.2%) |
| No | 262 (78.2%) | 1,104 (94.4%) | 1,366 (90.8%) |
| Antihypertensive drugs usage, n (%) | |||
| Yes | 428 (68.7%) | 0 (0.0%) | 428 (68.7%) |
| No | 195 (31.7%) | 0 (0.0%) | 195 (31.7%) |
| Aspirin usage, n (%) | |||
| Yes | 208 (33.5%) | 244 (12.8%) | 452 (17.9%) |
| No | 412 (66.5%) | 1,666 (87.2%) | 2,078 (82.1%) |
| Statin usage, n (%) | |||
| Yes | 158 (25.5%) | 38 (2%) | 196 (7.8%) |
| No | 462 (74.5%) | 1,866 (98%) | 2,328 (92.2%) |
The state with the most participants was Chiapas (12.9%), followed by Puebla (12.8%) and Sonora (11.9%). On the other hand, states with the smallest screened samples were San Luis Potosí (1.0%), Nuevo León (1.1%), and Zacatecas (2.0%). The highest mean BP standardized for age and sex was that of Coahuila (SBP 130.13 mmHg, DBP 85.20 mmHg) and the lowest that of Aguascalientes (SBP 110.75 mmHg, DBP 70.56 mmHg), as shown in Table 2. Stratifying by the SGI, states with a low SGI had the most participants (33.7%), and those with very low SGI had least participation (11.2%). Mean BP standardized by age and sex was highest at high SGI (SBP 124.14 mmHg, DBP 82.29 mmHg) and lowest at low SGI (SBP 121.14 mmHg, 78.64 mmHg), as can be seen in Table 3. The number of identified cases of hypertension decreased by 1.25% and 3.57% with the second and third readings, respectively, and increased to 5.18% using the mean of the three readings, as shown in Table 4.
Table 2.Mean Blood Pressure by State, before and after standardization by age and sex.
| State | n (%) | SBP (mmHg) | DBP (mmHg) | Standardized by age and sex | |||||
|---|---|---|---|---|---|---|---|---|---|
| SBP (mmHg) | DBP (mmHg) | ||||||||
| Mean | SD | Mean | SD | Mean | SD | Mean | SD | ||
| Aguascalientes | 154 (6.1) | 114.66 | 12.13 | 73.08 | 9.48 | 110.75 | 12.13 | 70.56 | 9.48 |
| Baja California | 160 (6.3) | 121.64 | 14.07 | 75.64 | 11.06 | 119.57 | 14.07 | 74.67 | 11.06 |
| Chihuahua | 176 (6.9) | 120.41 | 11.95 | 79.89 | 10.72 | 118.99 | 11.95 | 78.79 | 10.72 |
| Chiapas | 328 (12.9) | 119.89 | 11.58 | 76.91 | 8.26 | 118.78 | 11.58 | 76.97 | 8.26 |
| Coahuila | 104 (4.1) | 129.93 | 20.42 | 84.92 | 11.98 | 130.13 | 20.42 | 85.20 | 11.98 |
| Durango | 152 (6.0) | 122.16 | 14.82 | 82.09 | 22.54 | 118.62 | 14.82 | 80.88 | 22.54 |
| Guanajuato | 151 (5.9) | 114.71 | 7.99 | 75.44 | 5.06 | 114.21 | 7.99 | 75.34 | 5.06 |
| México | 167 (6.6) | 119.65 | 14.58 | 78.52 | 10.71 | 118.27 | 14.58 | 77.99 | 10.71 |
| Nayarit | 178 (7.0) | 120.04 | 11.91 | 79.55 | 9.33 | 118.64 | 11.91 | 78.88 | 9.33 |
| Nuevo León | 28 (1.1) | 122.75 | 6.94 | 77.14 | 3.20 | 122.04 | 6.94 | 76.95 | 3.20 |
| Puebla | 327 (12.8) | 124.43 | 14.36 | 76.64 | 8.05 | 123.13 | 14.36 | 76.33 | 8.05 |
| San Luis Potosí | 25 (1.0) | 123.47 | 15.37 | 80.51 | 11.28 | 114.85 | 15.37 | 76.58 | 11.28 |
| Sonora | 304 (11.9) | 122.71 | 14.60 | 80.93 | 12.02 | 120.82 | 14.60 | 79.73 | 12.02 |
| Veracruz | 240 (9.4) | 121.85 | 15.54 | 76.13 | 11.42 | 120.81 | 15.54 | 76.04 | 11.42 |
| Zacatecas | 51 (2.0) | 123.15 | 14.82 | 81.46 | 9.73 | 122.52 | 14.82 | 80.86 | 9.73 |
Mean Blood Pressure by Social Gap Index, Before and After Standardization by Age and Sex.
| Social Gap Index | n (%) | SBP (mmHg) | DBP (mmHg) | Standardized by age and sex | |||||
|---|---|---|---|---|---|---|---|---|---|
| SBP (mmHg) | DBP (mmHg) | ||||||||
| Mean | SD | Mean | SD | Mean | SD | Mean | SD | ||
| Very lowa | 286 (11.2) | 118.90 | 17.81 | 76.51 | 12.16 | 122.84 | 17.81 | 79.01 | 12.16 |
| Lowb | 858 (33.7) | 119.82 | 14.02 | 78.32 | 11.34 | 121.14 | 14.02 | 78.64 | 11.34 |
| Mediumc | 481 (18.9) | 117.24 | 12.07 | 78.40 | 14.31 | 120.07 | 12.07 | 80.98 | 14.31 |
| Highd | 352 (13.8) | 122.55 | 14.57 | 76.34 | 8.30 | 124.14 | 14.57 | 82.29 | 8.30 |
| Very highe | 568 (22.3) | 119.63 | 13.42 | 76.58 | 9.73 | 120.89 | 13.42 | 80.64 | 9.73 |
Mean Blood Pressure by Social Gap Index, Before and After Standardization by Age and Sex.
| Reading | SBP (mmHg) | DBP (mmHg) | Number with hypertension | Proportion of hypertension (%) | ||
|---|---|---|---|---|---|---|
| Mean | SD | Mean | SD | |||
| 1 | 120.43 | 15.29 | 77.50 | 11.23 | 546 | 21.45 |
| 2 | 119.21 | 14.67 | 77.37 | 18.24 | 514 | 20.20 |
| 3 | 119.05 | 14.15 | 77.26 | 11.37 | 455 | 17.88 |
| Mean of 1 and 2 | 119.82 | 14.50 | 77.43 | 12.74 | 450 | 17.68 |
| Mean of 2 and 3 | 119.13 | 14.12 | 77.31 | 12.73 | 422 | 16.58 |
| Mean of 1, 2 and 3 | 119.56 | 14.18 | 77.38 | 11.40 | 414 | 16.27 |
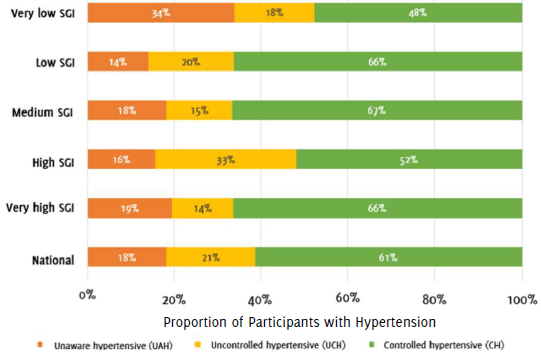
National mean BP, considering all three readings, was 119.56 mmHg for SBP and 77.28 for DBP. Classifying participants by type of case, as previously described, it was found that 922 (75.5%) were NH and 623 (24.5%) participants had hypertension. Of those with hypertension, 510 (81.9%) subjects had a previous diagnosis of hypertension, and only 82 (16.1%) did not declare taking a pharmacological treatment at the time of screening; 397 (61%) were CH patients, 128 (21%) were UCH patients and 113 (18%) were UAH cases. The proportion of UAH patients in areas with a very high SGI was only 1% above the national figure; meanwhile those areas with a very low SGI doubled it (34% vs. 18%). States with a low SGI were the areas with the smallest number of cases of UAH (14%). A high SGI was found to have the highest number of UCH cases (33%), being the only group of states surpassing the national figure. On the other hand, areas with medium SGI had the largest proportion of CH cases (67%). In contrast, regions with a very low SGI had the smallest proportion of controlled patients, followed by the states with low SGI, 13% and 9% below the national figure, respectively, as shown in Figure 2.
Figure 2Proportion of Unaware, Uncontrolled and Controlled Hypertensives by Social Gap Index.
The most common medications among participants were antihypertensive drugs, such as angiotensin-converting enzyme inhibitors (ACEIs), angiotensin receptor blockers (ARBs), calcium channel blockers, diuretics, beta-blockers, and alpha-agonists, with 428 (16.8%) patients taking at least one of them, which accounted for 68.7% of hypertensive patients taking medication. Of these, 225 (52.6%) took one medication with 171 (76.0%) controlled, 145 (33.87%) took two medications and 98 (67.6%) were controlled, 42 (9.8%) took three antihypertensive drugs with 30 (71.4%) controlled, 10 (2.3%) took four different medications with 100% control rate, and 6 (1.42%) took five or more medications achieving BP control in 4 (66.7%). Aspirin was the second most used drug among hypertensive patients (33.5%), followed by statins (25.5%).
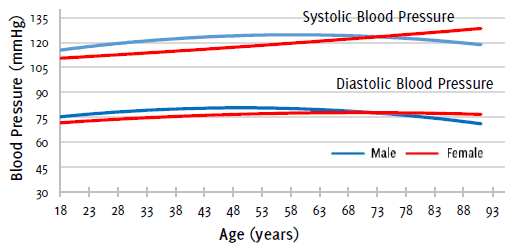
A polynomic (two degrees) model of the association between age and mean BP from all three readings, including patients not receiving pharmacological treatment, (Figure 3) showed an ascending linear trend for SBP in women, and an inverted U shape for DBP, with the largest increment in BP between 65 and 75 years of age. Meanwhile, both curves showed an inverted U shape for men with the highest BP levels between 50 and 60 years for SBP, and between 45 and 55 years for DBP. Men had an SBP higher than women up until 73 years, at which point trends are inverted. The same phenomenon was also observed for DBP at age 72.
Figure 3Change in Blood Pressure with Age and Sex from Linear Polynomic Model.
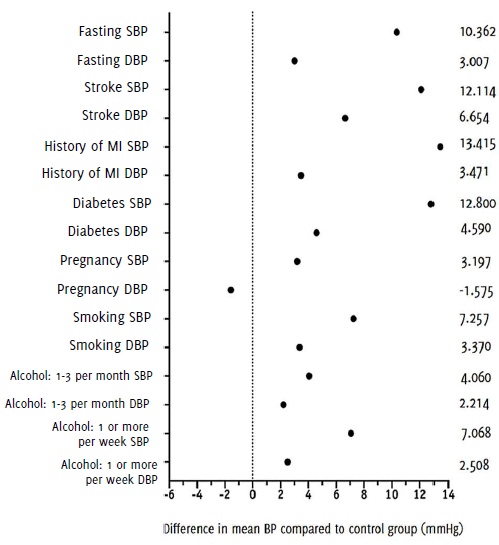
The control group was composed of 704 participants; their mean BP including all three readings was 114.52 mmHg for SBP and 75.14 mmHg for DBP. Analyzing for possible factors attributable to changes in BP, all variables except pregnancy, which decreased DBP by 1.5 mmHg, were associated with an increased mean difference (MD) in BP, as can be seen in Figure 4. Factors with the most influence over SBP were history of MI (13.41 mmHg), diabetes (12.80 mmHg), and stroke (12.11 mmHg). The highest increase in DBP was observed in participants with a history of stroke (6.64 mmHg), diabetes (4.59 mmHg) and MI (3.47 mmHg). Tobacco smoking was shown to increase SBP by 7.25 mmHg and DBP by 3.37 mmHg, whereas alcohol drinking increased 4.06 and 7.06 mmHg for SBP and 2.21 and 2.50 mmHg for DBP in those who drank one to three times per month and at least once a week, respectively. Aside from medical history, fasting at the time of screening was the condition associated with the highest increase in SBP (10.36 mmHg); DBP only increased by 3.01 mmHg.
Figure 4Change in Mean Systolic and Diastolic Blood Pressure Compared to Non-hypertensives for Associated Factors to Changes in Blood Pressure.
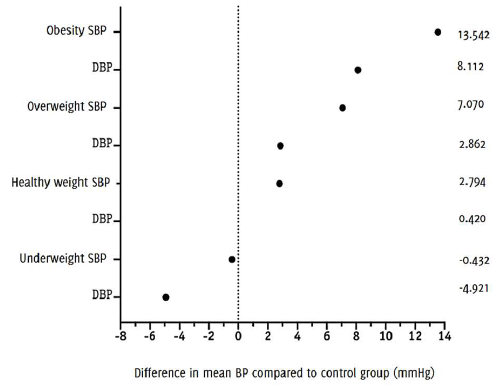
A proportional increase in BP and BMI was observed, with obese participants having an additional 13.54 mmHg in SBP and 8.11 mmHg in DBP. On the contrary, those considered underweight had a decrease of 0.43 mmHg in SBP and 4.92 mmHg in DBP compared with those in the control group, as shown in Figure 5.
Figure 5Change in Mean Systolic and Diastolic Blood Pressure Compared to Non-hypertensives, for Body Mass Index Category.
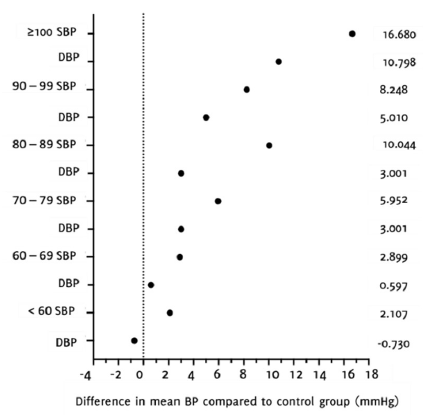
Comparing mean heart rate from all three BP readings, a similar phenomenon from that observed with BMI emerges, where the greater the heart rate, the higher the increase in BP. An increase of 16.68 mmHg in SBP and 10.79 mmHg in DBP were seen with heart rates ≥100 bpm. Meanwhile, when the heart rate is <60 bpm, DDB descends 0.73 mmHg (see Figure 6) compared to the control group.
Figure 6Change of Systolic and Diastolic Blood Pressure Compared to Non-hypertensives, for Heart Rate Range.
In this study of over 2,500 adults in Mexico, it was observed that 24.5% were hypertensive, similar to the 25.5% reported by the ENSANUT 2016 study and lower compared to 73.0% reported by the MMM 2019 study for the Americas region.6,10 Of those with hypertension, 18.0% were unaware they might have it, 21.0% were uncontrolled hypertensives and 61.0% had BP values <140/90 mmHg, therefore were considered to be well-controlled patients for this study. These numbers are far more optimistic than those reported by previous studies with only 45.6% and 37.1% of controlled subjects and 40.0% and 53.5% of unaware patients in national and global surveys, respectively.10,12 This could be explained by the opportunistic nature of this study. Also, through this campaign, hypertension awareness was raised in only 113 individuals across Mexico.
According to Ríos-Blancas et al.,13 low and very low SGI states have a higher probability of receiving a pharmacological treatment than states with a high and very high SGI, which accounts for three in four cases receiving treatment, but less than a third of these achieving BP control. This is consistent with the findings in this study, which showcased that states with a high marginalization were found to be the largest contributor to the pool of uncontrolled cases (33%). On the other hand, the largest proportion of hypertension unawareness was observed at very low SGI states (34%), almost doubling the national figure. In contrast, states with medium (67%), low, and very high SGI (66%) had the highest proportion of controlled hypertensives. Possible explanation for this could be that limited access to medications adds to their perceived value among populations that are not accustomed to receiving medical treatment, which improves compliance in these groups.
More than half of the participants taking antihypertensive agents were on a single medication, achieving blood pressure control in almost 8 in 10 patients. This is the largest proportion compared with the use of additional medication in this study, which contrasts with the findings of the MMM 20196 where almost 4 in 10 patients on a single agent were uncontrolled. However, these findings do not dispute the recommendations to initiate pharmacological treatment with two agents14,15 as a 67.6% controlled rate was observed with this regimen. The questionnaire used in this study did not allow to collect data about specific types of antihypertensive drugs used by participants, only the number of pharmacologic agents they used. On the other hand, aspirin was taken by a large proportion of participants, 33.5% of hypertensives and 12.8% of non-hypertensives, which goes against the latest recommendations about minimizing the routine usage of aspirin for the primary prevention of CVD because of lack of net benefit.16
A strong association consistent with previous publications was observed between BP and several known risk factors such as smoking and alcohol intake,17,18 with the latter showing a dose-response effect with a greater increase in BP in heavy drinkers similar to what has been described by other authors.19 A higher BMI was consistently related to a higher BP, although participants considered to have obesity in this study had a much higher increase in BP (SBP 13 mmHg and DBP 8 mmHg) compared to that reported by previous studies.6,19,20 This is a serious concern because Mexico has one of the highest rates of obesity worldwide, and these are continuing to rise,21 therefore a similar trend in hypertension could be expected if no further actions are taken.
On the other hand, subjects with a history of stroke and MI showcased a surplus in BP compared to the control group with an increase of 12 and 13 mmHg in SBP, respectively. A similar phenomenon was also observed in people with diabetes. These findings could suggest that patients with a history of stroke and MI in this population were not adequately controlled, even though hypertension is the most important factor for stroke recurrence.22 However, a J-curve phenomenon has been described23 in which a permissible BP target should be achieved to prevent the overly strict controlling of BP increasing the risk of adverse outcomes. On the contrary, evidence suggests that prompt, long-term BP control is imperative to improve secondary prevention of MI.24 Thus, further studies are needed to explore this topic, specifically in the Mexican population.
Risk of ascertainment and selection bias were inherent to the design because participants presented voluntarily at screening sites; therefore, people worried about their BP were more likely to participate. Thus, prevalence should not be inferred. It is worth noting that standardized by age and sex mean BP was within the normal range in all states. Coahuila had the highest mean BP with 130/85 mmHg, whereas Aguascalientes had the lowest with 110/70 mmHg. As an opportunistic campaign and cross-sectional study using convenience sampling, it could be expected that a higher proportion of health-conscious individuals (either well-controlled hypertensive patients or otherwise healthy people) took part in the study, which could explain atypical results. Any generalization about these results should be made cautiously.
Despite efforts to provide training on standardized BP readings to volunteers, differences in screening locations, and the usage of different equipment account for some degree of error in measurements. Although data about the devices used to measure BP was collected, the heterogeneity in reporting and the vast array of brands and models did not facilitate further analysis. However, as reported by Varshney et al.,25 there is no significant difference in BP readings using automated and auscultatory methods to determine SBP in the context of a community-based screening program, but DBP might differ between methods. Likewise, the main researchers did not have control over the number of students working at screening sites, which further limits the accuracy of measurements.
Most current guidelines recommend using ambulatory or home BP measurements,14,15 this approach was not cost-effective for this study, and the diagnosis of hypertension was based on a single set of readings. While this might not be ideal, spaced serial measurements including three BP readings provided a means to mitigate the impact of atypical values, errors in measurement or factors related to the patient such as white coat syndrome. On the other hand, at least one BP reading was missing for 31.4% of participants, which could significantly affect the statistical analysis and lead to an over-diagnosis of hypertension. Using multiple imputation, it was possible to mitigate that error by estimating mean second and third BP readings from a single measurement with minimal error in data distribution models. Nevertheless, the interpretation of results from this imputed data should be taken carefully.
A questionnaire was used to obtain the medical history of participants. This limits our ability to explore other comorbidities not included in the original questionnaire, but it does not mean that other associations with hypertension (apart from diabetes, MI, and stroke) could not be found. Also, this questionnaire asked participants about the usage of pharmacological agents prescribed by a physician for BP control, thus, differences in the accuracy of recollection could have led to a recall bias involving the number of drugs taken by participants.
To our knowledge, this is currently the only medical student-led campaign to raise hypertension awareness at a national level in Mexico. It was observed that a significant proportion of the study population was unaware of having hypertension, especially in states with a lower level of marginalization and considered to be more developed. In contrast, a larger number of subjects within BP control targets were found in more marginalized, less developed regions.
Most uncontrolled hypertensive patients in Mexico belong to marginalized states. These results could inform state legislative policy to help bridge these healthcare gaps by improving hypertension detection, especially among those who do not partake in regular health checkups or have limited access to healthcare.
The authors would like to thank Sara Patricia Yee-González, Eliezer Morales-Rojas, Andrea Isabel Ochoa-Rodríguez, Jonathan Dazaeth Delgado-Sánchez, Manuel Antonio Moreno-Colorado, Edson Lezama-Cisneros, Sandra Juárez-Paredes, José Arturo Valdés-Méndez and all the Asociación Mexicana de Médicos en Formación, A.C. members who served as volunteers at screening sites.
The Authors have no funding, financial relationships or conflicts of interest to disclose.
Conceptualization, Funding Acquisition, Project Administration, Resources, Supervision: JAYM, SANR. Data Curation, Validation: JAYM. Formal Analysis: SRP. Investigation: JAYM, SANR, SRP, JCGR, MMR. Methodology, Visualization: JAYM, SANR, SRP. Writing – Original Draft Preparation: JAYM, SANR, SRP, JCGR, MMR. Writing – Review & Editing: JAYM, SANR, SRP.
1. McEvoy JW, Daya N, Rahman F, Hoogeveen RC, Blumenthal RS, Shah AM, et al. Association of Isolated Diastolic Hypertension as Defined by the 2017 ACC/AHA Blood Pressure Guideline with Incident Cardiovascular Outcomes. JAMA. 2020 Jan 28;323(4):329-38.
2. Schwalm JD, McCready T, Lopez-Jaramillo P, Yusoff K, Attaran A, Lamelas P, et al. A community-based comprehensive intervention to reduce cardiovascular risk in hypertension (HOPE 4): a cluster-randomised controlled trial. Lancet. 2019 Oct 5;394(10205):1231-42.
3. Beaney T, Schutte AE, Tomaszewski M, Ariti C, Burrell LM, Castillo RR, et al. May Measurement Month 2017: an analysis of blood pressure screening results worldwide. Lancet Glob Health. 2018 Jul;6(7):e736-43.
4. Yusuf S, Joseph P, Rangarajan S, Islam S, Mente A, Hystad P, et al. Modifiable risk factors, cardiovascular disease, and mortality in 155-722 individuals from 21 high-income, middle-income, and low-income countries (PURE): a prospective cohort study. Lancet. 2020 Mar 7;395(10226):795-808.
5. Zhou B, Danaei G, Stevens GA, Bixby H, Taddei C, Carrillo RM, et al. Long-term and recent trends in hypertension awareness, treatment, and control in 12 high-income countries: an analysis of 123 nationally representative surveys. Lancet. 2019 Aug 24;394(10199):639-51.
6. Beaney T, Schutte AE, Stegiou GS, Borghi C, Burger D, Charchar F, et al. May Measurement Month 2019: The Global Blood Pressure Screening Campaign of the International Society of Hypertension. Hypertension. 2020 Aug;76(2):333-41.
7. Ruilope LM, Chagas AC, Brandao AA, Gómez R, Alcalá JJ, Paris JV, et al. Hypertension in Latin America: Current perspectives on trends and characteristics. Hipertens Riesgo Vasc. 2017 Jan-Mar;34(1):50-56.
8. Sudharsann N, Geldsetzer P. Impact of Coming Demographic Changes on the Number of Adults in Need of Care for Hypertension in Brazil, China, India, Indonesia, Mexico, and South Africa: A Modeling Study. Hypertension. 2019 Apr;73(4):770-76.
9. Sahoo D, Gosai H, Sahoo U, Harsoda JM. Awareness and Practices of Non-Pharmacological Approaches for Management of Hypertension in a Geriatric Population. Int J Med Students. 2014 Jun 17;2(2):53-55.
10. Campos I, Hernández L, Pedroza A, Medina C, Barquera S. Hypertension in Mexican adults: prevalence, diagnosis and type of treatment. Ensanut MC 2016. Salud Publica Mex. 2018 May-Jun;60(3):233-43.
11. National Council for Evaluation of Social Development Policy. Social Gap Index 2015: Results presentation. Available from: https://www.coneval.org.mx/Medicion/Documents/Indice_Rezago_Social_2015/Nota_Rezago_Social_2015_vf.pdf. Last updated May 2016; cited June 24, 2020.
12. Chow CK, Teo KK, Rangarajan S, Islam S, Gupta R, et al. Prevalence, Awareness, Treatment, and Control of Hypertension in Rural and Urban Communities in High-, Midle-, and Low-Income Countries. JAMA. 2013 Sep 4;310(9):959-68.
13. Ríos-Blancas MJ, Cahuana-Hurtado L, Lamadrid-Figueroa H, Lozano R. Effective coverage of treatment of hypertension in Mexican adults by states. Salud Publica Mex. 2017 Mar;59(2):154-64.
14. Williams B, Mancia G, Spiering W, Rosei EA, Azizi M, Burnier M, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension: The Task Force for the management of arterial hypertension of the European Society of Cardiology (ESC) and the European Society of Hypertension (ESH). J Hypertens. 2018 Oct;36(10):1953-2041.
15. Whelton PK, Carey RM, Aronow WS, Casey DE, Collins KJ, Himmelfarb CD, et al. ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults. A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines 2017. Hypertension. 2018 Jun;71(6):e13-115.
16. Arnett DK, Blumenthal RS, Albert MA, Buroker AB, Goldberg ZD, Hahn EJ, et al. 2019 ACC/AHA Guideline on the Primary Prevention of Cardiovascular Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2019 Sep 10;74(10):1376-1414.
17. Narkiewicz K, Maraglino G, Biasion T, Rossi G, Sanzuol F, Palatini P. Interactive effect of cigarettes and coffee on daytime systolic blood pressure in patients with mild essential hypertension. J Hypertens. 1995 Sep;13(9):965-70.
18. Gordon T, Kannel WB. Drinking and its relation to smoking, BP, blood lipids, and uric acid. The Framingham study. Arch Intern Med. 1983 Jul;143(7):1366-74.
19. Beany T, Burrell LM, Castillo RR, Charchar FJ, Cro S, Damasceno A, et al. May Measurement Month 2018: a pragmatic global screening campaign to raise awareness of blood pressure by the International Society of Hypertension. Eur Heart J. 2019 Jul 1;40(25):2006-17.
20. Landi F, Calvani R, Picca A, Tosato M, Martone AM, Ortolani E, et al. Body Mass Index is Strongly Associated with Hypertension: Results from the Longevity Check-Up 7+ Study. Nutrients. 2018 Dec 13;10(12):1976.
21. Devaux M, Graf S, Goryakin Y, Cecchini M, Huber H, Colombo F. The Organisation for Economic Co-operation and Development: Obesity Update 2017. Available from: https://www.oecd.org/els/health-systems/Obesity-Update-2017.pdf. Last updated 2017; cited June 24, 2020.
22. Castilla-Guerra L, Fernandez-Moreno MC. Chronic Management of Hypertension after Stroke: The Role of Ambulatory Blood Pressure Monitoring. J Stroke. 2016 Jan;18(1):31-37.
23. Ohta Y, Tsuchihashi T, Ibayashi S, Matsumura K, Kitazono T, Ooboshi H, et al. Blood Pressure Control in Hypertensive Patients With a History of Stroke. J Stroke Cerebrovasc. 2005 Nov-Dec;14(6):229-33.
24. Konstantinou K, Tsioufis C, Koumelli A, Mantzouranis M, Kasiakogis A. Doumas M, et al. Hypertension and patients with acute coronary syndrome: Putting blood pressure levels into perspective. J Clin Hypertens. 2019 Aug;21(8):1135-43.
25. Varshney VP, Harrison T, Szymczakowski M, Grossi M, Jones C. Developing a Protocol for Medical Student-Organized Community-Based Hypertension Screening Programs. Int J Med Students. 2013 Apr 30;1(1):8-11.
José Adrián Yamamoto-Moreno, 1 Physician, Universidad Autónoma de Baja California, Facultad de Medicina y Psicología, Tijuana, México
Suzzette Anaís Navarro-Rodríguez, 2 Medical student, Universidad de Sonora, Departamento de Medicina y Ciencias de la Salud, Hermosillo, México
Samuel Ruiz-Pérez, 3 Medical student, Universidad Autónoma de Baja California, Facultad de Medicina y Psicología, Tijuana, México
Juan Carlos Godínez-Reyes, 4 Medical student, Universidad de Guadalajara, Centro Universitario de Ciencias de la Salud, Guadalajara, México
Marvin Mendoza-Rojo, 5 Medical student, Universidad Autónoma de Chihuahua, Facultad de Medicina y Ciencias Biomédicas, Chihuahua, México
About the Author: José Adrián Yamamoto-Moreno is a recently graduated physician from a 7-year program at Universidad Autónoma de Baja California in México. He was awarded the Carlos Slim Foundation scholarship for excellence in Medicine and served as National Officer of Medical Publications in Asociación Mexicana de Médicos en Formación (AMMEF) from 2019-2020.
Correspondence: Jose Adrián Yamamoto-Moreno. Address: Avenida Alvaro Obregon s/n, Nueva, 21100 Mexicali, B.C., Mexico. Email: adrian.yamamoto@uabc.edu.mx
Editor: Francisco J. Bonilla-Escobar Student Editors: Madeleine J. Cox, Lakshmimathy Subramanian Copyeditor: Leah Komer Proofreader: Nicole Katherine Conners Layout Editor: Annora A Kumar
Cite as: Yamamoto-Moreno JA, Navarro-Rodríguez SA, Ruiz-Pérez S, Godínez-Reyes JC, Mendoza-Rojo M. Hypertension Awareness, Treatment and Control in Mexico: An Opportunistic Medical Student-led Blood Pressure Screening Campaign – A Cross-Sectional Study. Int J Med Students. 2020 Sep-Dec;8(3):263-9.
Copyright © 2020 José Adrián Yamamoto-Moreno, Suzzette Anaís Navarro-Rodríguez, Samuel Ruiz-Pérez, Juan Carlos Godínez-Reyes, Marvin Mendoza-Rojo
This work is licensed under a Creative Commons Attribution 4.0 International License.
International Journal of Medical Students, VOLUME 8, NUMBER 3, December 2020