Herpes-Zoster distribution.
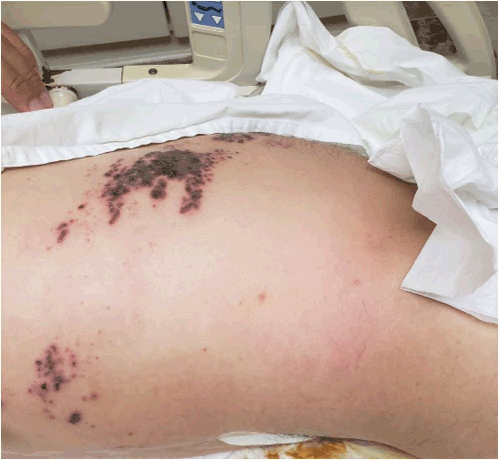
Legend: Vesicles and erythema in a dermatomal distribution (T8-10) associated with the clinical symptomatology established the clinical diagnosis of herpes zoster in this patient.
Victor A. Novelo-Hernández1, Marco Cárdenas2, Claudia Torres-González1, Patricio García-Espinosa1, Rómulo Ramírez2, Marco Díaz-Torres2, Alejandro Marfil-Rivera2
doi: http://dx.doi.org/10.5195/ijms.2021.863
Volume 9, Number 3: 227-230
Received 01 12 2020: Rev-request 27 12 2020: Rev-request 04 03 2021: Rev-request 21 06 2021: Rev-recd 27 12 2020: Rev-recd 09 03 2021: Rev-recd 14 07 2021: Accepted 09 08 2021: Publication 12 08 2021
ABSTRACT
Abstract Background:Myelitis post Herpes-Zoster is a rare condition that is typically associated with immunocompromised states. It usually starts as an acute loss of sensory and motor functions below the affected spinal cord level. The condition can range in severity from a mild to a fatal presentation. Other neurological complications include meningitis, atypical presentations should encourage the search for undiagnosed immunosuppression states.
The Case:We describe the case of a 42-year-old man, with previously undiagnosed HIV, who developed acute myelitis and meningitis after the appearance of the classic zoster lesions. On lumbar puncture and subsequent CSF analysis, the patient was found to have Froin's Syndrome. The patient was initiated with ceftriaxone, vancomycin, and acyclovir regimen and prophylactic antiphymic treatment was also added. After 14 days in the hospital, the fever, headache, and neck stiffness subsided while the sphincter function and lower limb paraplegia did not improve.
Conclusion:Varicella zoster virus reactivation suggests underlying immunosuppression. This case demonstrates the importance of being cognizant to the wide range of clinical manifestations that may suggest spinal cord involvement after clinical reactivation. Furthermore, physicians also need to be mindful that Acquired Immunodeficiency Syndrome (AIDS) and other immunodeficiency states could present with atypical clinical manifestations.
Keywords: Immunosuppression; Myelitis; HIV; Acquired Immunodeficiency Syndrome; Varicella-Zoster Virus Infection; Herpes Zoster (Source: MeSH-NLM).
Varicella-Zoster Virus (VZV) is a highly infectious, exclusively human virus with worldwide prevalence. Primary infection of VZV leads to acute varicella, and after primary infection, the virus is established on a cranial nerve and dorsal root ganglia with a lifelong latency.1 Reactivation leads to Herpes Zoster (HZ) which presents as an exanthem of vesicular lesions in a dermatomal distribution and is highly painful. HZ is an opportunistic infection with an increased risk in patients who are immunocompromised.1 However, the incidence of HZ has decreased in HIV/AIDS patients since the introduction of antiretroviral therapy (from 2,955 per 100,000 in 1992-1996 to 628 per 100,000 between 2009 and 2011).2 Neurological complications secondary to HZ can occur, with meningitis being the most frequent.3
Myelopathy is a less common neurological complication secondary to HZ, with an estimated incidence of less than 1 per 1,000 cases, and affects most often immunocompromised patients or older patients in general, representing less than 0.3% among the patients with HZ virus infection.4
The onset of HZ myelitis is usually acute or subacute, usually occurring after two weeks of vesicular rash appearance.4 The pathophysiology is still unknown, but tissue findings include inflammation with mononuclear infiltration and microglial proliferation, hemorrhagic necrosis, and degeneration of motor and sensory roots.4 Additionally, cellular immunity deficits seen in AIDS may lead to a fatal form of myelitis, spinal cord infarction, or progression of the disease and involvement of the diaphragm.5 Commonly, it presents as a mild and self-limited syndrome, but the spinal cord can become severely inflamed and cause serious complications such as recurrent HZ myelitis, loss of sensation and ability to ambulate, bacterial superinfection, postherpetic neuralgia, and fatal myelitis that is mostly seen in immunocompromised patients.6,7
Highlights:
- Post-herpes zoster myelitis is a very uncommon presentation.
- This case presents the importance of screening for undetected HIV infections.
- Introduction of clinical and images to improve curiosity about the case.
Froin's syndrome is defined by the presence of xanthochromia (yellow or pink color), the elevation of protein levels (>500 mg/dl), and hypercoagulation state on CSF cytology, and is an unusual condition that is presented after irritation and blockage of CSF (usually due to a mass or abscess). The combination of these three signs is considered pathognomonic; due to the effect on the spinal cord, the neurologic examination could expose paralysis of the lower limbs, decreased sensation, and other components of myelopathy.8
Here, we present the case of an AIDS patient with meningitis and severe myelitis due to VZV reactivation, with a less described presentation, and this also represents one of the few reported cases that developed Froin's syndrome.
The reported cases of Froin's syndrome, in the context of a CNS invasion by VZV, are mostly related to encephalitis, with only one case associated with myelitis. VZV myelitis usually presents in more advanced age, as in the case presented by Kleinschmidt-DeMaster et al., wherein 2016 they presented the case of a 54-year-old man with a known history of several comorbidities.9 In our case, the patient was healthy before, as he was only known to have high blood pressure and was diagnosed with HIV after the onset of the symptomatology.9
A 42-year-old man complaining of burning constant pain with distribution in T8-T10 dermatome was admitted to the emergency department. The pain did not radiate and did not have any aggravating nor relieving factors. The pain started 10 days before his admission, in the aforementioned dermatomes, with the subsequent appearance of vesicles and erythema in the same zone (Figure 1). The oppressive holocranial headache appeared 72 hours before admission, with occipital predominance, and was accompanied by symptoms of fever, vomiting, urinary retention, and lower limb weakness. The patient has a history of systemic arterial hypertension, alcoholism, and an exploratory laparotomy with cystography 20 years ago secondary to abdominal trauma.
Figure 1.Herpes-Zoster distribution.

On examination, there was moderate paraparesis (3/5 Medical Research Council scale, MRC) and neck stiffness, with the rest of the exam unremarkable. These findings raised the suspicion of a central nervous system (CNS) infectious process, so the patient underwent a cranial simple computed tomography (CT), lumbar puncture, viral panel. Empiric treatment for meningitis was initiated (ceftriaxone 2g IV q12h, vancomycin 1g IV q8h, acyclovir 750 mg IV q8h).
The viral panel was performed and positive for HIV-1 and the cluster of differentiation 4 (CD4) count was markedly low (104 cells/uL). The CT scan showed no pathological changes, but the lumbar puncture demonstrated xanthochromia, pleocytosis with lymphocyte predominance, hyper proteinorachie (1430 mg/dl), hypoglycorrhachia (21 mg/dl), and hypercoagulation, consistent with viral meningitis and Froin's Syndrome. BioFire® meningitis/encephalitis panel was performed with a positive result for VZV. Because of the condition, coinfection with bacteria or mycobacteria could not be ruled out, so anti-Tuberculosis treatment (doTBal®) was added, and cultures for fungi and mycobacteria were obtained. A GeneXpert® MTB/RIF test was run with a negative result. GeneXpert® MTB/RIF is a real-time polymerase-chain-reaction-based (RT-PCR) method used for rapid and accurate detection of active tuberculosis and to determine resistance for rifampicin. The decision was made to discard extrapulmonary tuberculosis as an etiological agent or tuberculosis as a coinfection (tuberculosis is considered endemic in the author's state). RT-PCR performed to detect the presence of VZV resulted positive.
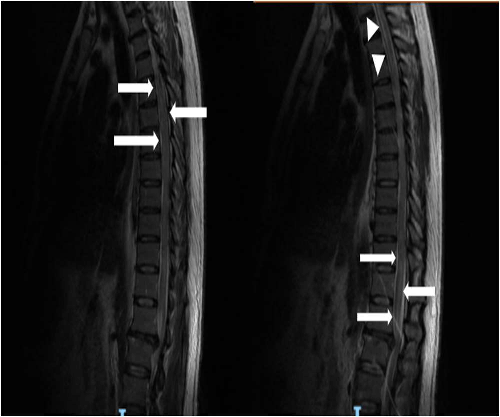
On the second day of hospitalization, the patient developed bowel incontinence and an increase in the lower limb weakness (2/5 MRC) with anesthesia. This raised the suspicion of inflammatory myelitis and treatment with methylprednisolone was initiated (1 g IV q24h for 5 days). Magnetic resonance imaging (MRI) of the dorsal spine was performed, showing a widened spinal cord at T4–T7 levels, with hydrosyringomyelia above this level (T1–T4) and a T2 weighted hyperintensity zone near the conus medullaris (T11-L1). This established the diagnosis of acute transverse myelitis (Figure. 2 A, B).
Figure 2.Magnetic Resonance Imaging.
After 14 days in the hospital and treatment with ceftriaxone, vancomycin, acyclovir and, doTbal®, the patient was discharged with outpatient follow-up. The fever, headache, and neck stiffness subsided, but sphincter function and lower limb paraplegia did not improve.
This case report was about disseminating how atypical clinical symptoms of myelitis are in patients with HZ reactivation, in addition to the complications that these reactivations can have on a patient's lifestyle as a result of not improving after treatment.
Post HZ myelitis and meningitis are rare but very well described CNS complications.9 The infection of the meninges has a clinical presentation easy to recognize and is more common than myelitis in the immunocompetent population.9,10
Besides being rarer than meningitis, the HZ myelitis tends to be harder to suspect due to the clinical presentation, which tends to be atypical in patients with decreased immune function.10 HZ myelitis usually manifests as an acute onset of sensory loss, focal weakness, and sphincter dysfunction (bladder dysfunction being more common than bowel) below the affected level.10
Immunocompromised patients tend to have atypical presentations of Herpes Zoster, even without the appearance of characteristic herpetic skin lesions, and may show a variation in the temporal relationship between these lesions and the medullary symptoms (usually 1–2 weeks).10 However, the frequency of topographic dissociation between the affected dermatomes and the level of the myelitis is not significantly different with immunocompetent patients.10 In this case, the patient presented with urinary retention (described more in sacral spine involvement) and bowel incontinence, two less common features but equally important to consider, especially if other typical symptoms do not appear.4
To confirm the diagnosis, VZV DNA and VZV IgG detection by real-time PCR and serology, respectively, are the methods of choice and must be done simultaneously.11 DNA decreases within the first 7 days of symptomatology start while antibodies increase proportionally.12 Serology must be measured on paired serum and CSF.12 The typical MRI findings include T2 hyperintensities and focal swelling, sometimes large enough to occlude the subarachnoid space, which, like in this case, caused Froin's syndrome, which is characterized by the triad of xanthochromia, elevation of protein levels (>500 mg/dL), and hypercoagulation state as well as the clinical manifestations of myelopathy.13,14 It is believed that the hypercoagulation state is responsible for starting a series of diffusion processes that lead to the aforementioned findings of Froin's syndrome.14,15 The reported cases of Froin's syndrome, in the context of a CNS invasion by VZV, are mostly related to encephalitis, with only one case associated with myelitis. However, none have been found to be associated with myelitis and meningitis simultaneously, which makes this case unique.5,16,17
Standard treatment has not been established, and some authors have proposed using acyclovir combined with a corticosteroid regimen, while others opt for the single use of antivirals, with differences and inconsistencies in the outcomes.8,9,14,15 This explains the need to carry out more specific studies that establish a treatment that improves the prognosis of these patients.
This case highlights the importance of focusing on the whole range of manifestations that may suggest a spinal cord involvement following Herpes Zoster reactivation. It shows the importance of suspecting this condition in immunocompromised patients, in whom the disease can cause excessive inflammation and progress rapidly towards a fatal outcome or important sequelae. In this specific context, it is necessary to be cognizant about multiple differential diagnoses with a wide range of possible etiological agents that can lead to confusion and delay in beginning a specific treatment may improve the clinical outcome.
Fernando Góngora-Rivera and Ingrid Estrada-Bellmann. Neurology Department professors who help us with comments.
Any relevant funding was received from any source for this manuscript.
Conceptualization: VAN, MD; Data Curation: VAN, CT, RR; Formal Analysis: VAN, MD; Funding, Methodology: RR; Investigation: MC, PG, RR, MD; Project Administration: VAN, MC, CT, PG, RR; Resources: MC, RR, MD, AM; Software: CT, PG, RR; Supervision: VAN, MC, CT, PG, RR; Validation: VAN, MC, CT, PG, RR; Visualization, Writing-Original Draft Preparation: VAN, MC, CT, PG, RR, MD, AM; Writing-Review and Editing: VAN, MC, CT, PG, RR.
1. Pergam SA, Limaye AP. AST Infectious Diseases Community of Practice. Varicella zoster virus (VZV) in solid organ transplant recipients. Am J Transplant. 2009 Dec;9 Suppl 4(Suppl 4):S108–15.
2. Grabar S, Tattevin P, Selinger-Leneman H, de La Blanchardiere A, de Truchis P, Rabaud C, et al. Incidence of herpes zoster in HIV-infected adults in the combined antiretroviral therapy era: results from the FHDH-ANRS CO4 cohort. Clin Infect Dis. 2015 Apr 15;60(8):1269–77.
3. Chamizo FJ, Gilarranz R, Hernández M, Ramos D, Pena MJ. Central nervous system infections caused by varicella-zoster virus. J Neurovirol. 2016 Aug;22(4):529–32.
4. Gilden D, Nagel MA, Cohrs RJ, Mahalingam R. The variegate neurological manifestations of varicella zoster virus infection. Curr Neurol Neurosci Rep. 2013 Sep;13(9):374.
5. Corti M, Trione N, Villafañe MF, Risso D, Yampolsky C, Mamanna L. Acute meningoencephalomyelitis due to varicella-zoster virus in an AIDS patient: report of a case and review of the literature. Revista da Sociedade Brasileira de Medicina Tropical. 2011 Oct;44:784–6.
6. Agrawal MM, Mahajan RS, Bilimoria FE, Ninama KR. Myelitis: A Rare Neurological Complication of Herpes Zoster. Indian J Dermatol. 2016 Nov;61(6):687–9.
7. Nakano T, Awaki E, Araga S, Takai H, Inoue K, Takahashi K. Recurrent herpes zoster myelitis treated with human interferon alpha: A case report. Acta Neurol Scand. 1992 May;85:372–5.
8. Dancel R, Shaban M. Images In Clinical Medicine. Froin's Syndrome. N Engl J Med. 2016 Mar 17;374(11):1076.
9. Kleinschmidt-DeMasters BK, Mahalingam R, Shimek C, Marcoux HL, Wellish M, Tyler KL, Gilden DH. Profound cerebrospinal fluid pleocytosis and Froin's Syndrome secondary to widespread necrotizing vasculitis in an HIV-positive patient with varicella zoster virus encephalomyelitis. J Neurol Sci. 1998 Aug 14;159(2):213–8.
10. Kim SH, Choi SM, Kim BC, Choi KH, Nam TS, Kim JT, Lee SH, Park MS, Kim SJ. Risk Factors for Aseptic Meningitis in Herpes Zoster Patients. Ann Dermatol. 2017 Jun;29(3):283–287.
11. Hung CH, Chang KH, Kuo HC, Huang CC, Liao MF, Tsai YT, Ro LS. Features of varicella zoster virus myelitis and dependence on immune status. J Neurol Sci. 2012 Jul 15;318(1-2):19–24.
12. Kedar S, Jayagopal LN, Berger JR. Neurological and Ophthalmological Manifestations of Varicella Zoster Virus. J Neuroophthalmol. 2019 Jun;39(2):220–231.
13. Noaillon M, Breining A, Greffard S, Sagot C, Verny M. Post-Herpes zoster myelitis in a very old patient: A complication not to be missed. Geriatr Gerontol Int. 2016 Jan;16(1):145–6.
14. Garispe A, Naji H, Dong F, Arabian S, Neeki M. Froin's Syndrome Secondary to Traumatic and Infectious Etiology. Cureus. 2019 Dec 6;11(12):e6313.
15. Greenfield JG. Original Papers: ON FROIN'S SYNDROME, AND ITS RELATION TO ALLIED CONDITIONS IN THE CEREBROSPINAL FLUID. J Neurol Psychopathol. 1921 Aug;2(6):105–41.
16. Kennedy PG. Issues in the Treatment of Neurological Conditions Caused by Reactivation of Varicella Zoster Virus (VZV). Neurotherapeutics. 2016 Jul;13(3):509–13.
17. Abbas SA, El Helou J, Chalah MA, Hilal H, Saliba G, Abboud H, et al. Longitudinal Extensive Transverse Myelitis in an Immunocompetent Older Individual-A Rare Complication of Varicella-Zoster Virus Reactivation. Medicina (Kaunas). 2019 May 23;55(5):201.
Victor A. Novelo-Hernández, 1 School of Medicine, Universidad Autónoma de Nuevo León, Monterrey. México.
Marco Cárdenas, 2 Neurology Service, “University Hospital “José Eleuterio González”, Universidad Autónoma de Nuevo Leon, Monterrey. México.
Claudia Torres-González, 1 School of Medicine, Universidad Autónoma de Nuevo León, Monterrey. México.
Patricio García-Espinosa, 1 School of Medicine, Universidad Autónoma de Nuevo León, Monterrey. México.
Rómulo Ramírez, 2 Neurology Service, “University Hospital “José Eleuterio González”, Universidad Autónoma de Nuevo Leon, Monterrey. México.
Marco Díaz-Torres, 2 Neurology Service, “University Hospital “José Eleuterio González”, Universidad Autónoma de Nuevo Leon, Monterrey. México.
Alejandro Marfil-Rivera, 2 Neurology Service, “University Hospital “José Eleuterio González”, Universidad Autónoma de Nuevo Leon, Monterrey. México.
About the Author: Victor Novelo is currently a fifth-year medical student of UANL medical school, Monterrey, Mexico. He is also first place of his medical generation.
Correspondence: Patricio García-Espinosa. Address: School of Medicine, Universidad Autónoma de Nuevo León, Monterrey. México. Email: patricio.garciaes@uanl.edu.mx
Editor: Shawn Albers & Francisco J. Bonilla-Escobar Student Editors: Adam Urback, Adnan Mujanovic, Brandon Belbeck & Purva Shah Copyeditor: Nguyen Tran Minh Duc Proofreader: Leah Komer Layout Editor: Sushil Dahal Process: Peer-reviewed
Cite as: Novelo-Hernández, VA, Cárdenas M, Torres-González C, García-Espinosa, P, Ramírez R, Díaz-Torres M, et al. A Case Report of Acute Severe Myelitis and Meningitis Secondary to Varicella Zoster Virus Reactivation in a Patient with Acquired Immunodeficiency Syndrome. Int J Med Students. 2021 Jul-Sep;9(3):227-30.
Copyright © 2021 Victor A. Novelo-Hernández, Marco Cárdenas, Claudia Torres-González, Patricio García-Espinosa, Rómulo Ramírez, Marco Díaz-Torres, Alejandro Marfil-Rivera
This work is licensed under a Creative Commons Attribution 4.0 International License.
International Journal of Medical Students, VOLUME 9, NUMBER 3, September 2021