Occupational Exposure to Blood and Body Fluids and Its Association with Anxiety Among Final-Year Medical Students: A Single-Center Cross-Sectional Study
DOI:
https://doi.org/10.5195/ijms.2026.3816Keywords:
Personal Protective Equipment, medical students, occupational exposure, clinical training, curriculum, anxietyAbstract
Background: Occupational exposure to blood and body fluids (BBFs) remains a significant risk for healthcare professionals, particularly those in training. These exposures not only pose a biological hazard but may also contribute to psychological distress. This study aimed to assess the prevalence of BBF exposure among final-year medical students and investigate its association with anxiety levels.
Methods: A cross-sectional study was conducted in January–February 2025 at Bursa Uludağ University Faculty of Medicine, Turkey. Of 271 final-year students, 203 participated (74.9%). Data were collected using a structured online questionnaire assessing sociodemographic characteristics, exposure history, and anxiety levels using the Generalized Anxiety Disorder-7 (GAD-7) scale. Predictors of anxiety severity were analyzed using negative binomial regression.
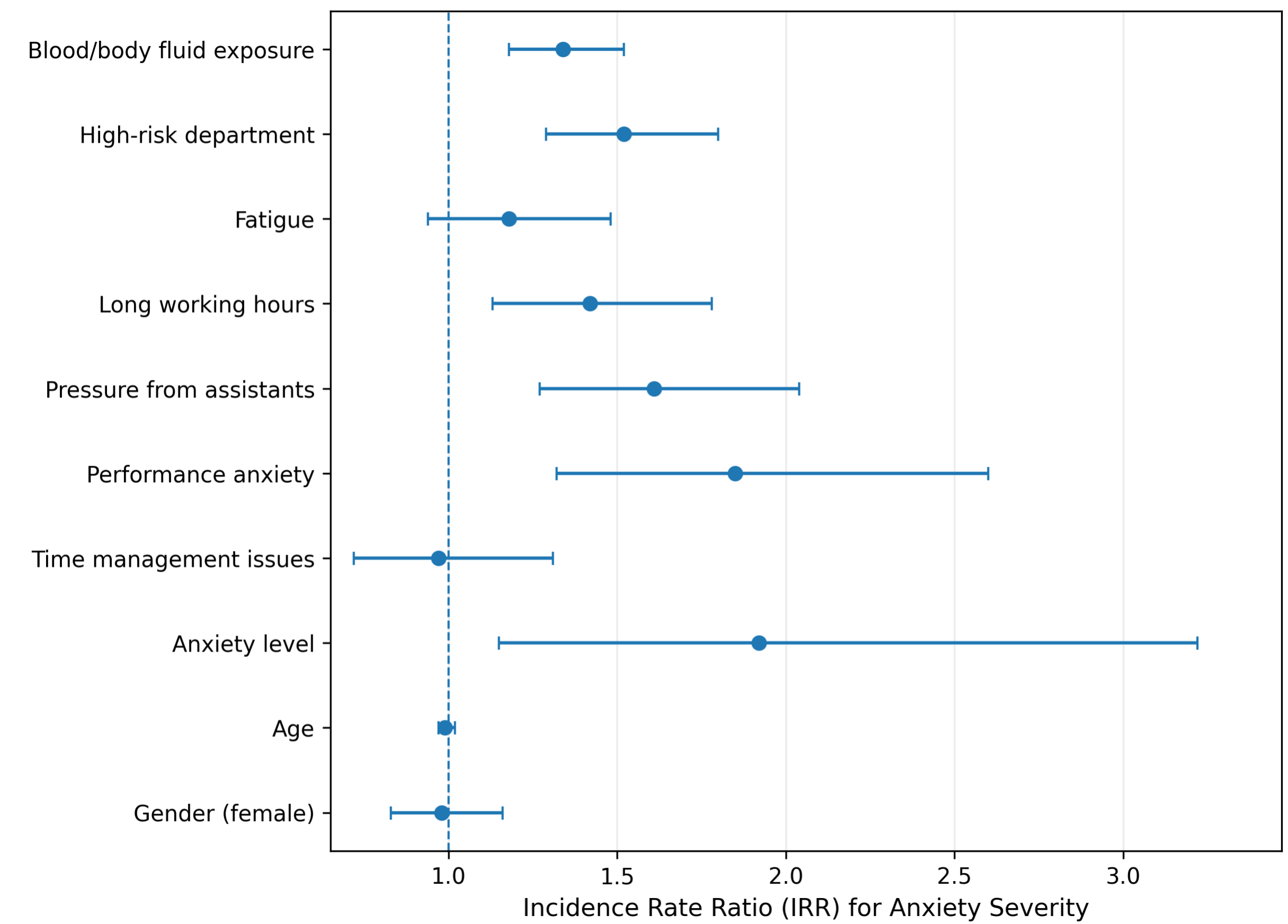
Results: Overall, 56.2% of students reported at least one BBF exposure, with 67.5% experiencing multiple incidents. Common exposures occurred during venipuncture (50%) and arterial puncture (33.3%), with emergency department rotations posing the highest risk (66.7%). Despite high glove usage (100%), gown usage was low (16.7%). The mean GAD-7 score was significantly higher among exposed students (7.21 vs. 5.39, p=0.016). Regression analysis revealed BBF exposure (IRR=1.34), high-risk departments (IRR=1.52), and factors like performance anxiety (IRR=1.85) significantly increased anxiety severity.
Conclusion: In this single-center study, occupational BBF exposure was highly prevalent among final-year medical students and was significantly associated with elevated anxiety levels, especially in high-pressure clinical settings. Despite existing safety training and orientations, the study's findings revealed persistent gaps in critical areas such as PPE compliance (low gown usage) and effective management of psychosocial stressors (hierarchical pressure).
References
1. Azap A, Ergönül O, Memikoğlu KO, Yeşilkaya A, Altunsoy A, Bozkurt GY, et al. Occupational exposure to blood and body fluids among health care workers in Ankara, Turkey. Am J Infect Control. 2005;33(1):48-52.
2. Puro V, De Carli G, Cicalini S, Soldani F, Balslev U; European Occupational Post-Exposure Prophylaxis Study Group. European recommendations for the management of healthcare workers occupationally exposed to hepatitis B virus and hepatitis C virus. Euro Surveill. 2005;10:260-264.
3. Prüss-Ustün A, Rapiti E, Hutin Y. Estimation of the global burden of disease attributable to contaminated sharps injuries among health-care workers. Am J Ind Med. 2005;48(6):482-490.
4. Osborn EH, Papadakis MA, Gerberding JL. Occupational exposures to body fluids among medical students: a seven-year longitudinal study. Ann Intern Med. 1999;130(1):45-51.
5. Triassi M, Pennino F. Infectious risk for healthcare workers: evaluation and prevention. Ann Ig. 2018;30(4 Suppl 1):48-51.
6. Zhang L, Ai Y, Liu J, Yue N, Xuan J, Bal V, et al. Economic burden of needle-stick injury among healthcare workers in China. Value Health. 2018;21:S86.
7. Erdem Y, Talas MS. Blunt and penetrating object injuries in housekeepers working in a Turkish university hospital. Am J Infect Control. 2006;34(4):208-214.
8. Gücük M, Karabey S, Yolsal N, Özden YI. İstanbul Tıp Fakültesi Genel Cerrahi Kliniği çalışanlarında kesici-delici alet yaralanmaları. Hastane Infeksiyonlari Dergisi. 2002;6(2):72-81.
9. Kişioğlu AN, Öztürk M, Uskun E, Kırbıyık S. Bir üniversite hastanesi sağlık personelinde kesici-delici yaralanma epidemiyolojisi ve korunmaya yönelik tutum ve davranışlar. Turkiye Klinikleri J Med Sci. 2002;22:390-396.
10. Moon CS, Hwang JH, Lee CS, Park KH, Kim ES. Exposure to blood and body fluid among medical students in Korea. Am J Infect Control. 2010;38(7):582-583.
11. Gaspar FW, Jolivet DN, Wizner K, Schott F, Dewa CS. Pre-existing and new-onset depression and anxiety among workers with injury or illness work leaves. J Occup Environ Med. 2020;62(10):e567-e572.
12. Granger S, Turner N. Work injuries and mental health challenges: a meta-analysis of the bidirectional relationship. Pers Psychol. 2025;78(1):11-57.
13. Spitzer RL, Kroenke K, Williams JBW, Löwe B. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166(10):1092-1097.
14. Konkan R, Şenormanci Ö, Güçlü O, Aydın E, Sungur MZ. Yaygın anksiyete bozukluğu-7 (YAB-7) testi Türkçe uyarlaması, geçerlik ve güvenirliği. Noropsikiyatri Ars. 2013;50(1):53-58.
15. Souza-Borges FRF, Ribeiro LA, Oliveira LCM. Occupational exposures to body fluids and behaviors regarding their prevention and post-exposure among medical and nursing students at a Brazilian public university. Rev Inst Med Trop Sao Paulo. 2014;56(2):157-163.
16. Inga E, López G, Kamiya C. Accidentes biológicos en estudiantes de medicina de una universidad peruana: prevalencia, mecanismos y factores de riesgo. An Fac Med (Lima). 2011;71(1):37.
17. Lee CS, Hwang JH, Seon SY, Jung MH. Exposure to blood and body fluids for medical students during clerkship. Korean J Med. 2008;74(5):500-505.
18. Alpat S, Özgüneş I, Nemli S, Erben N. Tıp fakültesi öğrencilerinde kan ve vücut sıvılarıyla temasa bağlı mesleki infeksiyon riski. Flora. 2008;13(2):88-92.
19. Karstaedt AS, Pantanowitz L. Occupational exposure of interns to blood in an area of high HIV seroprevalence. S Afr Med J. 2001;91(1):57-61.
20. Karani H, Rangiah S, Ross AJ. Occupational exposure to blood-borne or body fluid pathogens among medical interns at Addington Hospital, Durban. S Afr Fam Pract. 2011;53(5):462-466.
21. Cadman H, editor. WHO guidelines on drawing blood: best practices in phlebotomy. Geneva: WHO Press; 2010.
22. Aigbodion SJ, Motara F, Laher AE. Occupational blood and body fluid exposures and human immunodeficiency virus post-exposure prophylaxis amongst intern doctors. S Afr J HIV Med. 2019;20(1):958.
23. Lopes TL, Pinheiro AF, Silva CG, Mocelin PC, Zanin GD. Utilização, opinião e conhecimento dos profissionais de saúde sobre equipamentos de proteção individual durante a pandemia de SARS-CoV-2: um estudo transversal. Res Soc Dev. 2021;10(12):e26101220016.
24. Pereira A, Ribeiro A, Miranda G, Silva P, Silva A, Soares J, et al. Caracterização dos acidentes de trabalho num hospital terciário português entre 2017 e 2022. Rev Port Saude Ocup. 2023;15.
25. Roberts LW. Working together to ensure greater safety in our work and training environments. Acad Med. 2023;98(7):755-756.
26. Abere G, Yenealem DG, Wami SD. Occupational exposure to blood and body fluids among health care workers in Gondar Town, Northwest Ethiopia: a cross-sectional study. J Environ Public Health. 2020;2020:3640247.
27. Datar UV, Kamat M, Khairnar M, Wadgave U, Desai KM. Needlestick and sharps injury in healthcare students: prevalence, knowledge, attitude and practice. J Family Med Prim Care. 2022;11(10):6327-6333.
28. Quek TTC, Tam WWS, Tran BX, Zhang M, Zhang Z, Ho CSH, et al. The global prevalence of anxiety among medical students: a meta-analysis. Int J Environ Res Public Health. 2019;16(15).
29. Baxter AJ, Scott KM, Vos T, Whiteford HA. Global prevalence of anxiety disorders: a systematic review and meta-regression. Psychol Med. 2013;43(5):897-910.
30. Zhao LP, Kolonel LN. Efficiency loss from categorizing quantitative exposures into qualitative exposures in case-control studies. Am J Epidemiol. 1992;136:464-474.
31. Yaneva-Deliverska M. European Union regulation on prevention of sharps injuries in hospital and healthcare sector. J IMAB. 2012;18(3):357-359.
Published
How to Cite
License
Copyright (c) 2026 Levent Özdemir, Sena Sude Özyar, Sabrina İsrafilzade, Behrokh Khorasani

This work is licensed under a Creative Commons Attribution 4.0 International License.
Authors who publish with this journal agree to the following terms:
- The Author retains copyright in the Work, where the term “Work” shall include all digital objects that may result in subsequent electronic publication or distribution.
- Upon acceptance of the Work, the author shall grant to the Publisher the right of first publication of the Work.
- The Author shall grant to the Publisher and its agents the nonexclusive perpetual right and license to publish, archive, and make accessible the Work in whole or in part in all forms of media now or hereafter known under a Creative Commons Attribution 4.0 International License or its equivalent, which, for the avoidance of doubt, allows others to copy, distribute, and transmit the Work under the following conditions:
- Attribution—other users must attribute the Work in the manner specified by the author as indicated on the journal Web site; with the understanding that the above condition can be waived with permission from the Author and that where the Work or any of its elements is in the public domain under applicable law, that status is in no way affected by the license.
- The Author is able to enter into separate, additional contractual arrangements for the nonexclusive distribution of the journal's published version of the Work (e.g., post it to an institutional repository or publish it in a book), as long as there is provided in the document an acknowledgment of its initial publication in this journal.
- Authors are permitted and encouraged to post online a prepublication manuscript (but not the Publisher’s final formatted PDF version of the Work) in institutional repositories or on their Websites prior to and during the submission process, as it can lead to productive exchanges, as well as earlier and greater citation of published work. Any such posting made before acceptance and publication of the Work shall be updated upon publication to include a reference to the Publisher-assigned DOI (Digital Object Identifier) and a link to the online abstract for the final published Work in the Journal.
- Upon Publisher’s request, the Author agrees to furnish promptly to Publisher, at the Author’s own expense, written evidence of the permissions, licenses, and consents for use of third-party material included within the Work, except as determined by Publisher to be covered by the principles of Fair Use.
- The Author represents and warrants that:
- the Work is the Author’s original work;
- the Author has not transferred, and will not transfer, exclusive rights in the Work to any third party;
- the Work is not pending review or under consideration by another publisher;
- the Work has not previously been published;
- the Work contains no misrepresentation or infringement of the Work or property of other authors or third parties; and
- the Work contains no libel, invasion of privacy, or other unlawful matter.
- The Author agrees to indemnify and hold Publisher harmless from the Author’s breach of the representations and warranties contained in Paragraph 6 above, as well as any claim or proceeding relating to Publisher’s use and publication of any content contained in the Work, including third-party content.
Enforcement of copyright
The IJMS takes the protection of copyright very seriously.
If the IJMS discovers that you have used its copyright materials in contravention of the license above, the IJMS may bring legal proceedings against you seeking reparation and an injunction to stop you using those materials. You could also be ordered to pay legal costs.
If you become aware of any use of the IJMS' copyright materials that contravenes or may contravene the license above, please report this by email to contact@ijms.org
Infringing material
If you become aware of any material on the website that you believe infringes your or any other person's copyright, please report this by email to contact@ijms.org








